Asthma Is A Complex Condition
How do chest infections make asthma symptoms worse? | Asthma UK
Occasionally, people with asthma experience what are known as silent symptoms. This is where the signs of the tightening of the airways dont result in the familiar asthma sounds of wheezing and coughing. If you or someone you live with, work with, or care for experiences silent symptoms, it is important they consult a doctor for an ongoing Asthma Action Plan. People around the person with asthmasuch as co-workers, school teachers or daycare educators should know about the silent symptoms so they can respond if needed. Asthma can start at any age, and can be more of a problem when it starts in older adults. Dont assume if you never had asthma as a child that its not possible to develop symptoms now. Being breathless is not a normal part of getting older, it should always be checked out by a doctor. What Is Good Asthma CareYour doctor or nurse will tailor your asthma treatment to your symptoms. Sometimes you may need to be on higher levels of medication than at others. You should be offered:
It is also important that your GP or pharmacist teaches you how to properly use your inhaler, as this is an important part of good asthma care. What Causes Heaviness In Chest And ThroatIt is quite common for an individual to experience a sensation of heaviness in the chest and throat on an occasional basis. However, heaviness in the chest and throat can cause a lot of discomfort and interferes with routine activities of an individual. It is not always that this sensation is related to a cardiovascular condition but it is essential to rule out potentially serious medical conditions that may be causing heaviness in the chest and throat. Heaviness in the chest and throat happens when there is constriction in the throat and chest. There may be many causes for this to occur. Some of the causes of a feeling of pressure in the chest and throat are: Asthma: This is a medical condition in which the airways become narrow and swell as a result of secretion of mucous. This may result in tightness of the chest and throat. Additionally, the individual may find it difficult to breathe in cases of asthma which may further worsen the feeling of pressure in the chest and throat. Once asthma is treated the sensation of heaviness in the chest and throat gradually resolves. Respiratory System Disorders: This is yet another cause for sensation of pressure in the chest and throat. A respiratory system disorder can be caused due to allergies, inhaling contaminated air, and inhaling toxic chemicals. Bronchitis is the most common respiratory system disorder which tends to cause a sensation of heaviness in the chest and throat. Q: What Happens To The Lungs During A Mild Case Of CovidDr. Connolly: Once in the chest, the virus begins to impact a person’s airways causing inflammation. As inflammation increases, a barking, dry cough that sounds and feels like asthma develops. In addition, this can cause chest tightness or deep pain while breathing. Even though it’s generally mild for some people, the swelling and tightness that results from airway inflammation is essentially like having a sprained windpipe. Think of it like having a sprained ankle, but the effects and discomfort that come with having a sprain are felt inside of your chest. Ways To Reduce Chest Pressure When you are experiencing chest pressure and/or tightness, the key is to try to figure out the potential causes. Once you deem anxiety to be the cause of the symptom, the next goal is to stop it. See the following examples:
These are only temporary fixes. Remember that your chest pressure and/or tightness is often related to some type of anxiety issue or anxiety disorder. That means that the only way to prevent the chest pressure from returning is to learn to manage your anxiety. Q: What Happens To The Lungs During A More Severe Case Of CovidDr. Connolly: For some people, the infection becomes more serious and the lung tissue itself becomes swollen and filled with fluid and debris from dead cells which is clinically referred to as pneumonia. This fluid build-up can affect a person’s oxygen levels, and pneumonia can be mild, moderate, severe or even life-threatening, depending on how impaired gas transfer becomes and how difficult it is to breathe. If the transfer of oxygen into the blood stream is reduced, a person will often need supplemental oxygen and very close monitoring in a hospital setting. In very serious cases, a person may need to be placed on ventilator support in the ICU. Early on during the pandemic, there were a lot of unknowns about how contagious the virus could become during various medical interventions. Time and experience has taught us a lot about this virus, and now we’re able to more safely use several noninvasive breathing and oxygen devices, as well as techniques such as prone positioning before we have to resort to full life support with a ventilator. The Basics Of Diagnosing AsthmaYour doctor will probably start your examination by delving into your past medical history and asking whether any of your relatives have allergies or asthma. You’ll also be asked to describe your symptoms, their severity, and what, if anything, is triggering them. Triggers could include cold air, dust, hairsprays, perfumes, household cleaner vapors, cigarette or cigar smoke, and air pollution, Asciuto says. Doctors also try to narrow down the list of culprits by asking these additional questions:
Next, your doctor will listen to your breathing with a stethoscope and may order one or more of these diagnostic tests: Its also important to note that you can have asthma without experiencing any of the hallmark symptoms. There’s no single patient profile for asthma, says Dr. Fineman. “Some will have more coughing, some more wheezing, and some have more problems breathing with exercise, he says. Frightening Symptoms Of AnxietyChest tightness is an anxiety symptom that often causes a severe amount of distress. That is because chest tightness has a negative connotation that links it to severe health conditions. This can be very daunting for individuals who do not know much about the physical effects of stress and anxiety in their lives. Gerd And Heart Disease
Can Anxiety Cause Tightness In The Chest?
GERD can cause a  pain in your chest that can be confused with the symptoms of a  heart attack. Sometimes medical professionals diagnose GERD after evaluating a patient for episodes of chest pain that are found to be unrelated to heart disease. IMPORTANT! Never ignore pain in your chest. Seek immediate medical help. Call 911. Any delay in getting help may be fatal. If your doctor says you have GERD, ask what you should do when you have chest pain.  History And Physical ExaminationYour physical examination will include checking your vital signs, such as your temperature, pulse, and breathing rate. A fever can be an indication of an infection. Rapid breathing or a rapid heart rate can be a sign of a severe infection or an impending asthma attack. Your doctor will listen to your breathing sounds with a stethoscope, which will help determine whether your congestion is on one side of the lungs or both.
What You Can Do At HomeTo control or loosen mucus at home, you can try the following remedies: Drink lots of fluids. Drink plenty of water and other fluids, but not things that can dehydrate you, such as coffee and alcohol. Humidify. Try a cool mist humidifier or hop into a steamy shower to keep your airways moisturized. Dont smoke or vape anything. Whether from tobacco or marijuana, smoke is an irritant and can cause your body to make more mucus. Try a teaspoon of honey. Though honey doesnt get rid of mucus, it can calm your cough temporarily. Check air filters. Other irritants in the air can make mucus production worse, so make sure your heating and cooling system filters are clean and up to date. Take an expectorant. Some cough medicines contain guaifenesin, which loosens mucus so you can cough it up. Tips To Sleep Better With Severe Asthma At NightNocturnal asthma is associated with poor sleep quality. This condition of sleeplessness and its effects are worse for children. The average total sleep quality score of children affected by asthma is 51, which is above the clinical cut off of 41, but it indicates the pervasive sleep disturbances among this population. Here are a few tips that can help you sleep better with asthma at night: What Types Of Asthma Are There Healthcare providers identify asthma as intermittent or persistent . Persistent asthma can be mild, moderate or severe. Healthcare providers base asthma severity on how often you have attacks. They also consider how well you can do things during an attack. Asthma can be:
Functional Assessments Of Diseases That Masquerade As AsthmaShortness of breath, cough, wheezing and chest tightness are not specific for asthma. Thus children who present in this manner may have other medical conditions. The differential diagnosis of wheezing and dyspnea in pediatric subjects is influenced by the age of the patient. The younger the child, the more one has to consider congenital problems involving the airways or cardiopulmonary system. This is especially true for infants and toddlers. In terms of older children and adolescents, the confounding conditions will be more analogous to the problems seen in adults. When considering the possible causes, an assessment of lung function will often help arrive at the correct diagnosis. Children with bronchiolitis obliterans have experienced insults to their lungs that have led to scarring within small airways and severe airway obstruction.78 They may present with dyspnea and/or wheezing, leading to the impression that they have asthma. On assessment of lung function, they demonstrate an obstructive pattern with evidence of hyperinflation and decreased expiratory flow rates. The same pattern is seen in other obstructive processes, including asthma and cystic fibrosis. In bronchiolitis obliterans the correct diagnosis may be suggested by the lack of significant reversal of the airway obstruction with therapy that includes bronchodilators and/or corticosteroids, combined with other results such as lung imaging. In , 2016 Symptoms And Signs Of Bronchial AsthmaClassic bronchial asthma symptoms and signs* Bronchoconstriction caused by a CO2 deficiency* Inflammation of airways * Increased sensitivity of the immune system to innocent triggers * Excessive production of mucus in airways
Signs And Symptoms Of AsthmaTo establish a diagnosis of asthma, the clinician should determine that:
Recommended methods to establish the diagnosis are:
Additional studies are not routinely necessary but may be useful when considering alternative diagnoses: It is important to consider a diagnosis of asthma if certain elements of the clinical history are present they are not diagnostic by themselves but increase the probability of a diagnosis of asthma:
0 Comments
What To Do After An Asthma Attack
How does asthma work? – Christopher E. Gaw
An asthma attack can be a learning experience if you and your doctor use it to refine your asthma action plan. Get some tips on what to do after an asthma attack. An asthma attack is a sudden worsening of asthma symptoms that causes your air passages to become smaller and makes your breathing more difficult. Symptoms of an asthma attack may include difficult and painful breathing, coughing, and wheezing. Anyone with asthma needs to have a plan for what to do during an asthma attack. But you should also know what to do after an asthma attack. “You can’t always avoid an asthma attack, but you can check in with your doctor and use an asthma attack as a way to improve your asthma management,” said Jonathan Bernstein, MD, an associate professor in allergy and asthma at the University of Cincinnati Academic Health Center. “In some cases, an asthma attack may be an indication that you need to make some changes.” Seeing your doctor after an asthma attack is especially important if you are newly diagnosed. “Discussing the attack with your doctor can help you learn more about your asthma and empower you to manage your asthma better in the future,” said Sumita Khatri, MD, co-director of the asthma center at the Cleveland Clinic. What Asthma Treatment Options Are ThereYou have options to help manage your asthma. Your healthcare provider may prescribe medications to control symptoms. These include:
You can take asthma medicines in several different ways. You may breathe in the medicines using a metered-dose inhaler, nebulizer or other inhaler. Your healthcare provider may prescribe oral medications that you swallow. Is Fatigue A Sign Of AsthmaResponse from Leon C. Lebowitz, BA, RRT: Asthma is characterized by hypersensitivity of the airways. We tend to describe the main symptoms of asthma as coughing, wheezing, shortness of breath, and chest tightness, which may include pain or pressure.3 Waking up at night and concomitant fatigue are characteristics of poorly controlled asthma. Inadequate rest and sleep during the night subsequently impacts normal functioning during the day. Again, this may manifest itself as a feeling of being tired and/or feeling constantly exhausted.3 Persistent bouts of coughing combined with increased use of one’s accessory muscles during asthma exacerbations often results in muscle fatigue and sometimes, muscle pain. The constant wheezing that can accompany exacerbations also contributes towards a feeling of being weakened, tired, and fatigued.2 The best approach to treating the fatigue that is associated with one’s asthma is to keep it under control. Signs that asthma may be out of control include more frequent use of one’s rescue inhaler, increased shortness of breath, self-limiting physical activities because of one’s asthma condition, and any other signs that are specific for the individual.2 How Do You Monitor Asthma SymptomsMonitoring your asthma symptoms is an essential piece of managing the disease. Your healthcare provider may have you use a peak flow meter. This device measures how fast you can blow air out of your lungs. It can help your provider make adjustments to your medication. It also tells you if your symptoms are getting worse. After An Asthma Attack For several days following a flare-up you are at greater risk of additional asthma attacks. During this time period:
When you stray from your doctors orders regarding asthma treatment, you put yourself at risk of a serious condition called airway remodeling.
In this condition, your lungs become scarred. This reduces the effectiveness of your asthma medications and weakens your ability to breathe. You can avoid airway remodeling by working with your doctor to develop and maintain a treatment plan that works for you, reducing your risk of asthma attacks. If you need medical assistance, contact CareFinders at 1-866-608-FIND to make an appointment with a physician, or call 911 immediately if it is an emergency. What People With Asthma Need To Know About Face Masks During The CovidWe updated this blog post to include updated face mask guidance from the Asthma and Allergy Foundation of America and the Centers for Disease Control and Prevention . Face masks are an essential tool in our fight against COVID-19 . But wearing a face mask raises many questions for people with asthma. Do Children Need To Wear Face MasksCOVID-19 vaccines are now available in the U.S. for everyone 12 years old and older. Children in this age range should get vaccinated as soon as possible so they are protected from COVID-19. The CDC recommends universal indoor masking for all teachers, staff, students, and visitors to schools, regardless of vaccination status. Children with a disability that keeps them from safely wearing a mask and children under 2 should not wear masks. Book An Urgent Appointment With Your Gp Or Asthma NurseTell reception you need an urgent appointment because you’ve had an asthma attack. Book an appointment even if you feel better now. And even if youve been started on treatment for your asthma attack. Even if youre OK now you still need a check-up from your GP or asthma nurse to make sure youre not at risk from another attack. You need an urgent same day appointment if:
You need an urgent appointment within two working days if:
If you had an asthma attack but didn’t see your GP at the time it is still important to see your doctor or asthma nurse now, says Dr Andy Whittamore, Asthma UKs in-house GP. Your asthma may still not be well controlled and you could be at risk of another asthma attack. Recover more quickly from an asthma attack with support from your GPEven though you may have dealt with your asthma attack at home, or been treated for it in hospital, its still important to see your GP or asthma nurse after having an asthma attack. Your GP or asthma nurse can support your recovery and lower your risk of another attack. They can:check your medicines to see if youre on the best dose for you, and that youre taking your inhalers in the right way. When It Comes To Eosinophilic Asthma Severity Varies
What are the various triggers that can cause an asthma attack?
Symptoms of eosinophilic asthma can vary widely, according to Michael Peters, MD, an assistant professor of medicine in the division of pulmonary and critical care medicine at the University of California, San Francisco. Some patients describe an impact on daily life thats relatively mild, with just a little cough, Dr. Peters says. For others, its extremely debilitating where youre being treated in the hospital with high doses of corticosteroids and its completely changed your quality of life to the point that you cant really function at all. According to Parikh, some people with eosinophilic asthma experience a squeezing sensation in the chest. Many have a hard time taking deep breaths, or even catching their breath. Sometimes its so bad, people cant even talk, or cant talk in complete sentences. Other signs that point to eosinophilic asthma include ending up in the emergency room more, in the doctors office more, requiring higher doses of medicines requiring prednisone, says Parikh. People will say theyre unable to do simple household chores or play with their children, or they describe chest tightness like a squeezing pain that can sometimes be mistaken for a heart attack. Theyre missing work or school . Whats more, if you get woken up at night from your asthma, Parikh says, its a sign your asthma is uncontrolled. Remedies And Lifestyle FactorsAlthough medications can help control and treat symptoms, they are just one part of an effective treatment plan. A person should identify triggers and avoid them to help prevent future asthma attacks. Physical activity helps to 1 in 12 individuals in the United States. People with the condition have a lot of treatment and support options. People with nocturnal asthma should be on the lookout for signs of other related conditions, such as acid reflux and obstructive sleep apnea . These conditions have a bidirectional relationship with nocturnal asthma, which means that having one condition increases the chance of having the other. As many as of those with asthma also experience acid reflux. Some related conditions can be hard to spot. For example, nocturnal asthma and OSA have many of the same symptoms. If an individual thinks they may have OSA, they should contact their doctor. Managing nocturnal asthma is important for a persons health and quality of life. Nocturnal asthma can result in inadequate asthma control and increased morbidity, meaning a state of poor or decreasing health. According to the WHO, most deaths related to asthma symptoms occur during the night. Although asthma-related deaths are rare, they pose a real risk, so it is important that a person with asthma talk to a doctor and establish an effective treatment plan. Who Can Get AsthmaAnyone can develop asthma at any age. People with allergies or people exposed to tobacco smoke and secondhand smoke are more likely to develop asthma. Statistics show women tend to have asthma more than men, and asthma affects Black Americans more frequently than other races. When a child develops asthma, healthcare providers call it childhood asthma. If it develops later in life, its adult-onset asthma. Children do not outgrow asthma. They may have fewer symptoms as they get older, but they could still have an asthma attack. Your childs healthcare provider can help you understand the risks. How To Avoid Asthma TriggersIf you know what your asthma triggers are, then where possible, its beneficial to try to avoid them. If theres a particular allergen culprit you know of, then keeping your home clean and dust-free can help. For example, you could consider swapping carpets for wooden floors to reduce the amount of dust build-up or hiring a cleaner so youre not personally exposed to dust when cleaning. It can be more difficult to avoid asthma triggers completely when youre at work, especially if your asthma is occupational and linked to your working environment. In an ideal world, you could simply change jobs to something more suitable for your health, but in reality this isnt always feasible. Let your employer or the HR department know about your asthma. You should be able to discuss the options available for optimising your work environment to be more suitable to your needs. Keeping on top of your asthma management plan, working alongside your doctor or asthma nurse and making sure you take your inhalers or other asthma medications should help to control your symptoms. Making practical lifestyle choices is important too, like eating healthily, exercising and not smoking. It can also be beneficial to learn an asthma breathing technique. There are various breathing techniques that can help asthma and knowing how to breathe properly could help if something unexpectedly triggers an attack. What Are Asthma Attack Symptoms Usually is not terribly subtle, Dr. Grayson says. He explains that signs of an asthma attack often include:
These asthma attack symptoms can last a couple of hours for some people, he explains. In others, they might last for days. And some people die, Dr. Grayson says. Thats why anything thats limiting daily activities should be evaluated by your doctor right away. When people treat an attack as soon as it startsand take controller medicine to prevent attacks in the first placetheir risks reduce and outcomes improve, he says. Controller medications, often a corticosteroid, can be taken daily on a long-term basis to control underlying inflammation. They differ from rescue medications, like albuterol, which people take via an inhaler or nebulizer to open airways when they are experiencing asthma symptoms. What To Do During An Asthma AttackEveryone with asthma should have and follow a doctor-designed asthma action plan, says says Joi Lucas, MD, a pediatric pulmonologist and chief of pediatrics at Lakeland Regional Health in Lakeland, Florida. This personalized plan provides clear instructions for someones day-to-day asthma management. It also indicates what to do if symptoms worsensuch as during an attackclarifying measures like which medications to take and when to seek professional care. Dr. Lucas explains that these plans typically have three management sections that correlate with the severity of someones current symptoms, including:
An asthma action plan can also help people recognize the early warning signs of a serious attack, like feeling tired and out of breath, having an irritating cough, or developing cold or allergy symptoms. Why Asthma Can Wake You Up At NightIf your asthma isnt under control, you might get more symptoms at night. There are several reasons why this might happen:
If your GP has prescribed steroid pills for your asthma, youll probably be advised to take them in the morning after food, as they might cause difficulty sleeping if you take them at night, but always take them exactly as prescribed. Can People With Asthma Wear Face MasksYes, people with asthma can wear face masks. The CDC recommends that you wear a mask in public indoor spaces even if you are fully vaccinated. The WHO recommends wearing a fabric mask that allows you to breathe while talking and walking quickly. For people with very mild asthma or well-controlled asthma, its probably not going to be an issue, said Dr. David Stukus, member of the Medical Scientific Council for the Asthma and Allergy Foundation of America . For people who have very severe disease and have frequent exacerbations, ER visits, hospitalizations, require lots of medications and frequent symptoms, it might cause more issues for those folks. If youre having trouble wearing a mask, try a different fabric or fit. Wearing some kind of breathable face mask is better than nothing. According to the WHO, medical masks when worn the right way do not cause you to breathe in more carbon dioxide or reduce your oxygen levels. Other studies back this up as well. And a face mask made of three layers probably wont fit tightly enough to affect your oxygen either. If your mask is uncomfortable, try a new type of mask. The Relationship Between Asthma And Fatigue
What is an Asthma Attack? (Inflamed Airways)
Working hard to breathe requires a lot of energy. With asthma, there are many times you may be working hard without even realizing it, particularly if you have been living with this condition for a long time. You may be worried about how your illness is affecting you and your loved ones and the impacts it will have in the future. Stress is exhausting couple the stress of living with a chronic condition with the ordinary burdens of everyday life and its no wonder youre fatigued. Many people who suffer from asthma also are plagued with anxiety and depression. Both of these conditions drain your energy. Sleeplessness, medication and infections may cause fatigue as well. If your asthma fatigue is ongoing or difficult to relieve, consult with your health care provider. It could even be unrelated to your asthma, in which case it is very important you get to your doctors right away to determine treatment. Asthma Is A Complex ConditionOccasionally, people with asthma experience what are known as silent symptoms. This is where the signs of the tightening of the airways dont result in the familiar asthma sounds of wheezing and coughing. If you or someone you live with, work with, or care for experiences silent symptoms, it is important they consult a doctor for an ongoing Asthma Action Plan. People around the person with asthmasuch as co-workers, school teachers or daycare educators should know about the silent symptoms so they can respond if needed. Asthma can start at any age, and can be more of a problem when it starts in older adults. Dont assume if you never had asthma as a child that its not possible to develop symptoms now. Being breathless is not a normal part of getting older, it should always be checked out by a doctor. How Do You Stop An Asthma Attack Without An InhalerIf you are diagnosed with asthma, you should make sure you have an inhaler with you at all times. However, if a worst case scenario occurs and you experience when you dont have a reliever inhaler with you, there are practical steps you can take to ease your symptoms.
Asthma can be a life-threatening condition, so at the very least, aim to keep a spare reliever inhaler in your handbag, locker at work or coat pocket. What Are Other Benefits To Wearing Face MasksPollen can trigger asthma. Wearing a mask can help keep pollen from getting into your nose and lungs. Even though a mask can help prevent symptoms, consider going outside when pollen counts are lower. Changes in the weather can also be an asthma trigger, so keep it in mind when wearing a mask. When its cold, wearing a face mask can warm and humidify the air you breathe. Hot and humid weather can make wearing a mask more uncomfortable. Consider going out at times of the day when the weather is milder. Exercise is important for people with asthma. Stay active but avoid situations where you would need a mask. If you are outside on a trail or in a park, you probably wouldnt need to wear a mask. Consider working out outside or at home instead of going to a gym or exercise class that may require a mask. Masks also can protect you from respiratory infections like the flu, COVID-19, and even the common cold. Masks provide protection for people who are immunocompromised. What Should I Do If I Think I Have Asthma If you suspect you might have asthma, you should see your doctor for a professional diagnosis. Dont ignore it if you do have asthma, the sooner you get it under control, the faster you can get back to living a full and active life. For more information on how Asthma Australia is helping people with asthma to breathe so they can live freely, visit About Us. Nocturnal Asthma And ChildrenAsthma is more common in children than in adults and is the most common chronic disease in children worldwide. Accurately diagnosing and treating nocturnal asthma in children is especially important because the effects of nocturnal asthma, like loss of sleep and daytime sleepiness, are associated with behavioral and developmental difficulties. Unfortunately, nocturnal asthma often goes undiagnosed in children because they tend to underestimate or not report their nighttime symptoms. For this reason, its helpful for parents to monitor and report back to the doctor any concerning symptoms in children. These symptoms may include wheezing, disturbed sleep, daytime sleepiness, and difficulties concentrating at school. If You Suspect You Might Have Asthma Definitely Head To The DoctorYour doctor will probably give you a physical exam first to examine the general state of your health. After that, theyll likely put you through some lung function tests, such as a spirometry, which checks how much air you can exhale after taking a deep breath as well as how fast you can expel air, according to the Mayo Clinic. Or they may do a peak flow test, which measures how hard you can breathe out. If you cant exhale enough air or breathe out quickly, it may be a sign your lungs arent working well, which could point to asthma, Dr. Benzaquen says. There are other exams they can use, too, like exposing you to methacholine, a known asthma trigger, to see if your airways narrow, or allergy testing, since allergies and asthma are so often connected. If you are diagnosed with asthma, itll be within one of four categories, according to the Mayo Clinic. Mild intermittent asthma means you have minimal asthma symptoms for up to two days a week and up to two nights a month, while mild persistent asthma means youre experiencing symptoms more frequently than twice a week, but not more than once on any given day. Moderate persistent asthma ups the ante: Youre dealing with symptoms once a day and more than one night a week. Finally, severe persistent asthma involves constant symptoms most days and frequently at night too. Youre In Your FortiesThe peak years for the onset of asthma in adulthood are between 45 and 50, says Richard F. Lockey, MD, director of the Division of Allergy & Immunology at University of South Florida College of Medicine. Most at risk of developing symptoms of asthma are those who have allergies or those who suffered from the disorder as kids but thought they outgrew it. Many asthma symptoms start after an infection. You get a cold and suddenly you have asthma, Dr. Lockey says. Via https://www.knowyourasthma.com/can-an-asthma-attack-make-you-tired/ Can Asthma Lead To Copd Later
Asthma and COPD: Same or Different?
Not everyone with asthma goes on to develop COPD. However, having asthma as a child or younger adult can affect how well your lungs develop, and that can increase your chances of having COPD when youre older. One recent study reported that over one in 10 children with persistent asthma went on to have COPD as a young adult. This means that if you have asthma, its even more important that you dont smoke. Quitting will help to lower your chance of developing COPD in later life as well.Learn more about: Q: Whats The Difference Between Asthma And CopdAsthma occurs frequently in people with a family history of the disease and often begins in childhood. Symptoms include shortness of breath, wheezing, coughing, and chest tightness, and these symptoms flare up during an asthma attack. At other times, symptoms may fade or become minimal. COPD is different and usually strikes later in life. Most people diagnosed with COPD either used to smoke, or still do. Some symptomssuch as chest tightness and coughingare similar to asthma. Other symptoms, such as mucus production, are distinct to COPD. Unlike asthma, symptoms rarely ever fade completely. How Emphysema Relates To CopdEveryone whos diagnosed with emphysema is said to have COPD. However, its possible to be diagnosed with COPD and not have emphysema. A person can receive a COPD diagnosis while only having chronic bronchitis, for instance. Emphysema is usually the direct result of years of smoking cigarettes. Its symptoms tend to affect people who are middle-aged or older. Chronic bronchitis, which can occur earlier or later in life, can also be caused by tobacco smoking. Inflammatory Cells In CopdNeutrophils are present in sputum of smokers but increased in COPD and related to disease severity. They may be important in mucus hypersecretion and through release of proteases. Macrophages: big numbers are in airway lumen, lung parenchyma, and bronchoalveolar lavage fluid. They produce increased inflammatory mediators and proteases and may show defective phagocytosis. T lymphocytes: both CD4+ and CD8+ cells are increased in the airway wall and lung parenchyma, with big CD8+/CD4+ ratio. Increased is the number of CD8+ T cells and Th1 cells which secrete interferon- and express the chemokine receptor CXCR3. CD8+ cells may be cytotoxic to alveolar cells. B lymphocytes: are increased in peripheral airways and within lymphoid follicles, possibly as a response to colonization and infection. Eosinophils: increased eosinophil proteins in sputum and eosinophils in airway wall during exacerbations. Epithelial cells: May be activated by cigarette smoke to produce inflammatory mediators . Surgical Treatment For Copd If medical treatment does not alleviate the symptoms of COPD, or symptoms and exacerbations increase, surgery may be an option. However, in order to be a candidate for surgery, there are specific criteria. These include not being a current smoker, participating in a pulmonary rehabilitation program, and being strong enough to receive surgery. There are two types of surgery performed for COPD, Lung Volume Reduction Surgery and Bullectomy.
If damage to the lungs is too severe or surgery does not alleviate symptoms, a doctor may recommend a lung transplant. Are The Symptoms Of Asthma And Copd The SameAsthma and COPD can both cause wheezing, chest tightness, shortness of breath, and chronic cough. However, the frequency and predominating symptoms in asthma and COPD are different. With COPD, you are more likely to experience a morning cough, increased amounts of sputum, and persistent symptoms. If you have asthma, you are more likely to experience symptoms in episodes and/or at night. Additionally, asthma symptoms are likely to occur after exposure to specific triggers. Can Asthma Develop Into CopdOn occasion, some people with asthma have developed COPD. According to the American Lung Association, children who have severe asthma are more likely to develop COPD in adulthood than children who experience mild asthma. Studies show that more than 40 percent of children diagnosed with severe asthma developed COPD by age 50; these metrics may indicate a link between the disorders. Research is ongoing, and there is also speculation that children with severe asthma dont experience a faster decline in lung function in later adulthood, but perhaps lung development was compromised in early childhood. If this is true, it suggests that COPD can be prevented with better childhood asthma treatment. Asthma And Copd: What’s The Difference And Is There A LinkAsthma and chronic obstructive pulmonary disease are lung diseases. Both cause swelling in your airways that makes it hard to breathe. With asthma, the swelling is often triggered by something youâre allergic to, like pollen or mold, or by physical activity. COPD is the name given to a group of lung diseases that include emphysema and chronic bronchitis. Emphysema happens when the tiny sacs in your lungs are damaged. Chronic bronchitis is when the tubes that carry air to your lungs get inflamed. Smoking is the most common cause of those conditions . Asthma gets better. Symptoms can come and go, and you may be symptom-free for a long time. With COPD, symptoms are constant and get worse over time, even with treatment. Do Copd And Emphysema Have Different Causes
Long Case Presentation : COPD VS ASTHMA
Usually, COPD and emphysema can develop for the same reasons. The most common causes of all forms of COPD is cigarette smoking or exposure to secondhand smoke. Other causes of emphysema can include alpha-1-antitrypsin deficiency and inhaling toxic substances. Bronchiectasis may also have additional causes. It can develop as a result of certain inflammatory diseases, such as rheumatoid arthritis. Can You Have Asthma And Copd At The Same TimeBoth of these diseases affect airflow limitation, inflammation, and tissue remodeling, and it is possible to have both asthma and COPD at the same time. Older patients may have features of both diseases, leading to an overlap of the two conditions. Many people who have asthma and COPD will need to continue treatment to reduce the inflammation of their asthma, as well as manage the symptoms of their COPD to retain as much lung function as possible. As you age, the likelihood of overlap between these two diseases increases. Your physician will be able to confirm if you have both disorders and will be able to help you with treatment. The Differences Between Copd And Asthmaeditorial processSanja Jelic, MDMedical Review Board Asthma and chronic obstructive pulmonary disease are both respiratory diseases involving chronic inflammation that leads to airflow obstruction. While they share similar symptoms, their causes and treatments differ. In some cases, asthma and COPD may overlap in what is termed asthma-COPD overlap syndrome, or ACOS. However, the frequency and predominating symptoms in asthma and COPD are different. With COPD, you are more likely to experience a morning cough, increased amounts of sputum, and persistent symptoms. If you have asthma, you are more likely to experience episodic symptoms during and/or at night. Another difference between asthma and COPD is the intermittent symptoms seen with asthma versus the chronic, progressive symptoms seen in COPD. Asthma symptoms are likely to occur after exposure to specific triggers, whereas COPD symptoms occur more regularly. Copd Myth 1: A Copd Diagnosis Is A Death SentencePeople live a long time with COPD, Dr. Adams says. Especially now that we have many therapies that improve your chances of living longer with COPD. COPD never goes away, and its a progressive disease; but its one that can be managed, she adds. It requires that you do some things that may be really tough, like quitting smoking and getting plenty of exercise. But if you work closely with your healthcare team and follow your treatment plan, youll find that COPD is neither a death sentence nor a daily struggle. RELATED: 9 Tips to Help Slow the Progression of COPD Know About Asthmatic Bronchitis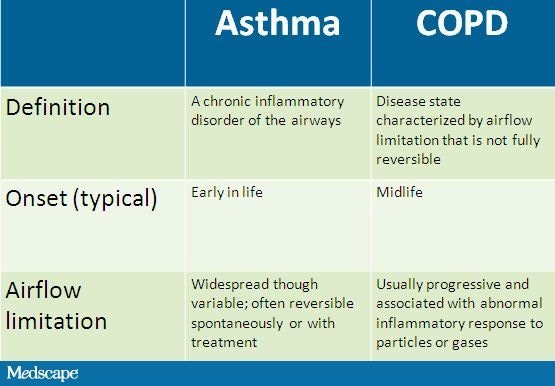 Asthma and bronchitis are defined as two inflammatory airway diseases. While they have distinct differences, as outlined above, asthma and acute bronchitis can occur together. This is known as asthmatic bronchitis. A number of factors can contribute to asthmatic bronchitis. What triggers the symptoms in one person may be different than what causes a flare-up in another; however, the following are the most common factors:
As you may have guessed, the symptoms of asthmatic bronchitis are a combination of asthma and bronchitis. They include shortness of breath, coughing, wheezing, tightness in chest and the production of phlegm. Due to a virus or bacteria bronchitis can be contagious, however chronic asthmatic bronchitis is not contagious. Respiratory diseases affect people of all ages- children, teens, adults and seniors. Most of these diseases, such as asthma, bronchitis and COPD, are chronic and all have a significant impact on the individual with the disease, as well as on family, the community and the health care system. Its in everyones interest to gain a better understanding of respiratory ailments, not only so current patients can breathe easier, but so that we can prevent future generations from suffering. Related Reading:Emphysema Vs Copd: Similarities And DifferencesIn some cases, there are a few differences between COPD and emphysema. Depending on the form of COPD a person has, symptoms may vary a little. For example, people with chronic bronchitis might have symptoms that differ slightly from people that have emphysema. Both conditions are classified as COPD, but symptoms may vary a little. But there are more similarities than differences between emphysema and COPD. For instance, the cause is often the same. Typically, COPD and emphysema occur due to damage to the airways, which makes breathing progressively more difficult. Is It Asthma Copd Or BothBoth asthma and chronic obstructive pulmonary disease , including emphysema and chronic bronchitis, make breathing difficult. In fact, they share many similarities. However, they are different lung diseases. Asthma-COPD overlap syndrome is diagnosed when you have symptoms of both asthma and COPD. ACOS is not a separate disease, but rather a way for doctors to recognize the mix of symptoms and select a treatment plan that is most appropriate for you. Copd Vs Asthma: What Is The DifferenceCOPD or chronic obstructive pulmonary disease and asthma are both chronic lung diseases. The most common cause of COPD is smoking, while asthma is an inflammatory response by the body. Symptoms of COPD worsen over time, but they can be treated and managed with drugs and other therapies. There is no cure for COPD. Some forms of asthma can be reversible with medication, drug therapies, and lifestyle changes. Both conditions can be life threatening. It’s Easy To Get The Care You Need
Distinguishing Between ASTHMA and COPD part 1
See a Premier Physician Network provider near you. Chronic obstructive pulmonary disease and asthma are often mistaken for one another. Thats understandable. These two lung diseases share some of the same symptoms: wheezing, chronic coughing and shortness of breath. To further cloud the distinction, about 40 percent of people who have COPD also have asthma. Asthma and COPD share some of the same risk factors such as smoking tobacco, exposure to air pollutants at home and work, genetics and respiratory infections. And asthma is considered a risk factor that increases the chances of developing COPD. But asthma and COPD are two distinct diseases. Here are two distinct differences.
A third difference is that COPD ranks high in third place on the Centers for Disease Control and Preventions list of leading causes of death, after heart disease and cancer.The good news is that with proper treatment, such as quitting smoking, airway-opening medications and avoidance of irritants and allergens, people with asthma and COPD can live more comfortably. What Is The Life Expectancy For Copd Vs Emphysema Are They FatalThe life expectancy can be estimated for COPD/emphysema by the BODE index previously mentioned. However, it is not possible to determine accurate life expectancy for these patients because of so many variables that may change. Nonetheless, types 3- 4 COPD/emphysema puts you at risk for many serious or fatal complications like pneumonia or heart failure. For this reason, some doctors consider types 3-4 COPD/emphysema to be a life threatening disease. Asthma Treatment Options&copd Treatment OptionsIn many cases, both lung diseases treatments are the same, such as Bronchodilators and inhalable steroids, but there are also a few treatment options that are specific to each condition.People with asthma may be encouraged to stay away from triggers or avoid going outdoors when pollen levels are high. In cases of people with severe asthma, a bronchial thermoplasty may be recommended. The procedure burns off some of the muscles in the airway, reducing their ability to constrict. On the other hand, people with COPD may be encouraged to alter lifestyle habits, such as quitting smoking, to help prevent any further damage. They may also be prescribed oxygen or pulmonary rehabilitation. In severe cases of COPD, procedures like lung volume reduction surgeries and lung transplants may be suggested. Both Asthma and COPD are treatable diseases that will require some lifestyle changes. Staying informed on your options and taking care of your health is very important in managing lung diseases. For any further questions about these conditions and their treatments, click the link below! Airflow Restriction: Reversible Or Permanent
Myth 3: Copd Is The Same Thing As Asthma While both are inflammatory conditions that cause coughing and wheezing, asthma and COPD are very different diseases, Adams says. About 15 percent of people can have both asthma and COPD, she notes. Dr. Carl agrees. Its not uncommon for people with COPD to also have some degree of asthma. While asthma can develop at any age, most people get asthma as children or teens. COPD develops slowly over time, and most people are 40 or older when symptoms become noticeable. Asthma can flare if youre exposed to allergens such as dust, pollen, or pet dander, but you can be symptom-free between episodes. People with COPD experience flares or exacerbations when they get a cold or an upper respiratory infection or are exposed to smoke or other lung irritants. Asthma is treated with long-term medications to reduce airway inflammation and quick-relief or rescue bronchodilators, as needed, for symptoms such as wheezing. COPD patients need to be on long-lasting inhalers as opposed to rescue medications, Adams says. Along with bronchodilators to widen the airways, some with COPD patients may benefit from anti-inflammatory drugs, such as steroids or anticholinergic agents to decrease mucus secretion and antibiotics to treat interval infections, adds Carl. RELATED: Your Breathe-Better Checklist for COPD Flares What Is The Difference Between Asthma And CopdAsthma is a respiratory disease affecting the bronchial tubes, or airways, making them sensitive to allergens or irritants, both of which can bring on an asthma attack. During an asthma attack, it is hard to breathe, and wheezing, coughing, and chest tightness may occur. While COPD can also cause these symptoms, its more likely to experience a consistent cough with phlegm. Unlike asthma, COPD is a chronic condition caused by damage to the lungs over time, most often from smoking, and it is irreversible. With asthma, breathing returns to normal after an attack, but COPD symptoms are more regular. Usually, COPD develops in people after age 40 and becomes a chronic disease of lung function while asthma may develop in people of almost any age. Q&a: When Youre Diagnosed With Both Asthma And CopdWhen youre diagnosed with asthma or chronic obstructive pulmonary disease , it can be difficult to breathe. But did you know that about 15% to 55% of adults with one of these lung diseases actually qualify for a dual diagnosis? This dual diagnosis is called asthma-COPD overlap syndrome . People at risk for ACOS are typically those with asthma who smoke, but healthcare providers also see cases in those who dont use tobacco. The right diagnosis is important with lung conditions, and education is key to understanding treatment options. To learn more about ACOS, read the answers to some common questions below. How To Score Your Copd Quiz:In the spaces below, write the number that is next to your answer for each of the questions. Add the number to get the total score. The total score can range from 0 to 10. ____+____ +____+____ +____ =________ TOTAL SCORE If your total score is 5 or more, this means your breathing problems may be caused by chronic obstructive pulmonary disease . The higher your score, the more likely you are to have COPD. COPD is often referred to as chronic bronchitis and/or emphysema and is a serious lung disease that slowly gets worse over time. While COPD cannot be cured, it is treatable, so please share your answers to the five question screener with your healthcare professional. Parade DailyIf your total score is between 0 and 4, and you are experiencing problems with your breathing, please share your answers to the five-question screener with your doctor or health care professional. Only your health care professional can decide if you have COPD. Your health care professional can help evaluate your breathing problems by performing a breathing test, also known as spirometry. Dont wait. Call your doctor today to make an appointment to see if you may be at risk for COPD. Remember, when speaking to your health care professional, be honest and open in describing your symptoms and explain how your breathing problems affect your activity level on a daily basis. Get more information on COPD at DRIVE4COPD. Who Can Get Asthma Or Copd
Bronchial Asthma & COPD
The most common risk factors for developing asthma is if you have a parent with asthma, or have had a severe respiratory infection as a child, or have an allergic condition, or have been exposed to certain chemical irritants or industrial dust in the workplace. Risk factors for COPD include:
Difference Between Asthma And BronchitisAbout 12 million people in the United States suffer from bronchitis every year. It is characterized by irritation of the mucous membranes lining the airways. Although there are similarities between asthma and bronchitis, they really arent the same disease and therefore require different treatments. During an asthma attack you will often find that in addition to having difficulty breathing, people will also wheeze. Many sufferers have also reported tightness in the chest. In the case of bronchitis, there is also normally a hacking cough. It can be with or without phlegm. Chronic bronchitis involves a persistent phlegm-producing cough. Chronic bronchitis can be diagnosed with a pulmonary function test. This will enable doctors to check airflow in the lungs. A chest x-ray can also be taken. Unfortunately, diagnosing asthma is more complex. It involves testing to check airway obstruction and a patients ability to exhale under various conditions. While asthma treatment focuses on limiting exposure to triggers and controlling inflammation, bronchitis treatment includes a number of different strategies. The flu vaccine, anti-inflammation treatments, antibiotics, and bronchodilators to open airways could be applied. There are also treatments that focus on helping to clear excess mucus. How Are They DiagnosedDiagnosing COPD or asthma starts with a comprehensive evaluation of your history. A provider will take into account factors such as:
Your doctor will also perform a physical exam, which includes:
However, the history and physical exam are often not enough to diagnose you with COPD or asthma. Your provider will probably want to do a few more tests before they make a diagnosis. The most useful to test to figure out if you have asthma or COPD is called spirometry. This test measures how much air you can breathe in and out of your lungs and how fast you can do it. You may be asked to do the test before and after taking an inhaled medication to see how your lungs respond. Your results are then compared to normal ranges based on your age, height, and sex. Chest X-ray or computed tomography scans are also common tests if you have trouble breathing. While the tests can show signs of pneumonia and other lung problems, they cant determine for certain whether you have COPD or asthma. Airway Remodelling And The Overlap SyndromeThere is also increased airway wall remodelling in the overlap syndrome, with increased bronchial wall thickening on high resolution CT . Increased thickness of the airway wall is an important feature leading to airway obstruction in most airway diseases. In asthma, this is due to inflammation, subepithelial fibrosis and increased thickness of the smooth muscle. There is also increased thickness of the airway wall in COPD, which is not as prominent as in asthma, but involves the same structures of the epithelium, reticular basement membrane, airway smooth muscle and mucous glands. There is also evidence of remodelling, fibrosis and inflammation in these structures. The increased smooth muscle reported in COPD is seen in some but not all studies. Increased thickness of the airway epithelium and goblet cell hyperplasia are features of the remodelled airway in both asthma and COPD. Similarly, increased airway wall fibrosis is reported in both asthma and COPD. Thus when considering the pathological changes within the airways that are associated with asthma and COPD, there is similarity in terms of structures that are remodelled, but differences in the degree of changes in specific structures. Inflammatory Mediators Involved In Asthma Chemokines are important in the recruitment of inflammatory cells into the airways and are mainly expressed in airway epithelial cells . Eotaxin is selective for eosinophils, whereas thymus and activationregulated chemokines and macrophage-derived chemokines recruit Th2 cells . Cysteinyl leukotrienes are potent bronchoconstrictors and proinflammatory mediators mainly derived from mast cells and eosinophils . Cytokines orchestrate the inflammatory response in asthma. Key cytokines include IL-1 and TNF, and GM-CSF. Th2-derived cytokines include IL-5, which is required for eosinophil differentiation and survival; IL-4, which is important for Th2 cell differentiation; and IL-13, needed for IgE formation . Histamine is released from mast cells and contributes to bronchoconstriction and inflammation . Nitric oxide , a potent vasodilator, is produced from syntheses in airway epithelial cells . Exhaled NO is increasingly being used to monitor the effectiveness of asthma treatment . Prostaglandin D2 is a bronchoconstrictor derived predominantly from mast cells and is involved in Th2 cell recruitment to the airways . Airway structural cells involved in the pathogenesis of asthma are: airway epithelial cells, airway smooth muscle cells, endothelial cells, fibroblasts and myofibroblasts and airway nerves . Via https://www.knowyourasthma.com/is-asthma-and-copd-the-same-thing/ Summary Of Recent Changes
Are asthma patients at greater risk from coronavirus?
Updates to the list of underlying medical conditions that put adults of any age at high risk for severe illness from the virus that causes COVID-19 were based on evidence from published reports, scientific articles in press, unreviewed pre-prints, and internal data. Updates to the following conditions were completed based on evidence from the date range below:
In keeping with an ever-growing volume of literature, references are now categorized by study type. With these categories, we can be more specific about the type of study used as supporting evidence. By presenting the references in these categories, clinicians can better evaluate the quality of the data to determine risk. Who Is Considered Clinically Extremely Vulnerable With AsthmaPeople are regarded as clinically extremely vulnerable if they are at very high risk of severe illness as a result of coronavirus , and may need to be admitted to hospital. People with asthma may be in this group if they have severe asthma or another condition that makes them clinically extremely vulnerable. Many children and young people who, at the start of the pandemic, were identified as clinically extremely vulnerable, have already been removed from the shielded patient list. The decision has now been made by the chief medical officer in all four UK nations to remove all remaining children and young people from the clinically extremely vulnerable list. Read more about children and the clinically extremely vulnerable list from our sister charity, the British Lung Foundation. Data has shown that age is by far the most important factor influencing a persons risk of becoming seriously ill with coronavirus. Its thought that although children can catch COVID-19, very few children develop severe symptoms, even if they have an underlying health condition. Are People With Asthma At Higher Risk Of Getting CovidSo, there is no hard evidence that people with asthma get sicker with COVID-19 . But is there any evidence that people with asthma are more likely to catch the coronavirus? Again, not that we are aware of. A study of 140 cases showed no link between coronavirus infections and asthma. Some people with asthma may wonder if they are immunocompromised and what that means. Immunocompromised means that your immune system is weakened, either by a disease or by a medication. It means you are more likely to catch an infection and more likely to have a more severe illness than someone who is not immunocompromised. Some people with asthma can be immunocompromised because of the medication they take. Here are some asthma medications and treatment combinations that can blunt the immune system:
Check with your provider if youre not sure about whether your medications could be making you immunocompromised. Study Finds No Evidence Patients With Asthma At High Risk For Adverse CovidDisclosures: We were unable to process your request. Please try again later. If you continue to have this issue please contact . A review of 150 studies yielded no clear evidence that patients with asthma are at increased risk for COVID-19 diagnosis, hospitalization, severity or mortality. Health agencies such as the CDC and WHO expressed the opinion that patients with asthma were more vulnerable to becoming severely ill with COVID-19, yet formal comprehensive assessments of the medical literature were lacking,Rajiv Dhand, MD, professor of medicine, Wahid T. Hanna MD Endowed Chair of Medicine and associate dean of clinical affairs at the Graduate School of Medicine at the University of Tennessee Health Sciences Center, told Healio. Patients with asthma were apprehensive about getting severe COVID-19 and wondered whether they should continue to use inhaled corticosteroids, which are the mainstays of asthma treatment. Am J Respir Crit Care Med Researchers identified 150 worldwide studies from PubMed and medRxiv databases by searching the terms asthma,SARS-CoV-2 and COVID-19 and cross-referenced citations in studies available in print or online before December 2020. Data on asthma prevalence were collected from studies of patients with COVID-19 and regional health statistics, and researchers compared asthma prevalence among patients with COVID-19 by region, disease severity and mortality. For more information:Rajiv Dhand, MD, can be reached at [email protected]. Steps Everyone Can Take To Lower The Risk Of Getting And Spreading Covid
Risk Of Severe Covid May Depend On Your Type Of Asthma Experts SayEveryone agrees about the good newsfolks whose asthma is spurred on by allergies don’t appear to have an increased risk of life-threatening illness if they contract COVID-19. “Asthma has not risen as one of the top comorbid diseases for worse COVID-19 outcomes,” said Dr. Sandhya Khurana, director of the Mary Parkes Center for Asthma, Allergy and Pulmonary Care at the University of Rochester Medical Center. “We always worry with asthma and viral infections, because they seem to trigger asthma exacerbation unreasonably. But what we’ve seen so far is reassuring.” But debate continues to swirl regarding the potential severity of COVID infection in people with non-allergic asthma. Some studies have suggested that people who have asthma caused by something other than allergiesexercise, stress, air pollution, weather conditionsmight have an increased risk of severe COVID-19. For example, Harvard researchers found that having non-allergic asthma increased the risk of severe COVID-19 by as much as 48%. That conclusion was based on data from 65,000 asthma sufferers presented in the June issue of the Journal of Allergy and Clinical Immunology. “For those people, I think being more cautious would be good for them,” said senior researcher Liming Liang, an associate professor of statistical genetics at the Harvard T.H. Chan School of Public Health in Boston. “I think the next wave is coming. We’ve got to be more cautious.” Explore further Free Advice For EveryoneAs a charity, Asthma UK provides free health advice to millions of people through our Website and our specialist nurses Helpline – a team dedicated to offering life-changing advice over the phone. As the UK’s leading asthma charity, now more than ever before people need our help, yet COVID-19 has devastatedour ability to raise vital funds! For us to continue being there for everyone who needs us, we need your support. If you’ve benefited from this advice on face coverings today, if you can please make a small donation to help ensure we can give you the support you need now and in the future. What Support Can I GetWherever you are in the UK, there is support available if you need to self-isolate. Find out more about support you can get if you are clinically extremely vulnerable. In all four nations, you can get in touch with your local COVID Mutual Aid group. Theyll put you in touch with people who live locally wholl be able to help you. In England, if you meet certain criteria, you can get support from the NHS volunteer responders. They can do things like helping you with shopping, getting prescriptions, or just checking in to see how you are doing. Register for support online or by calling 0808 196 3646. There are equivalent services in the devolved administrations. You might be entitled to welfare benefits. For more information on what you might be entitled to, take a look at our information or get in touch with the Citizens Advice Bureau . Tips For Wearing A Face Mask With Asthma
COVID-19 could be more severe in people with asthma
The Public Health Agency of Canada currently recommends that Canadians wear non-medical face masks while in public spaces where physical distancing cannot be maintained such as on public transit, or at the grocery store. Be sure to check your provincial or territorial authority for up-to-date guidance. Wearing a face mask is NOT a substitute for physical distancing or frequent handwashing. Wearing a non-medical face mask is an extra measure that can be taken to protect those around you. When worn properly, a person wearing a non-medical mask can reduce the spread of their own infectious respiratory droplets. Make sure you wear your mask properly. It should cover both your nose and mouth. If your mask gets soiled or wet, be sure to wash and dry it before wearing it again. You can read information about appropriate use of non-medical masks, and how to properly place, remove and clean a non-medical mask from the Public Health Agency of Canada. The vast majority of people with asthma can wear a non-medical mask safely. If you are unable to wear a non-medical mask without experiencing breathing issues, do not wear a mask. Instead, make sure you are practicing physical distancing by maintaining a 2-metre distance. Schedule an appointment with your healthcare provider as soon as possible to go over your Asthma Action Plan and review your asthma symptoms and control. Your healthcare provider may suggest or ask you to consider other options to protect yourself. Vulnerable Populations And CovidWhile COVID-19 can make anyone sick, some Canadians may be at greater risk of COVID-19 than others due to their occupational, social, economic and other health and life circumstances. Organizations, staff and volunteers play an important role in helping to prevent these populations from getting or spreading the COVID-19 virus. Start by sharing simple things they can do to help keep themselves and others healthy, guide them to help if they develop any signs and symptoms and learn ways help care for sick clients recovering from COVID-19. Covid No More Deadly For People With AsthmaHealthDay Reporter WEDNESDAY, Feb. 24, 2021 — During the pandemic, people with asthma have worried that their respiratory condition might raise their risk of severe illness or death from COVID-19, but new research findings should calm their fears. After analyzing data from 57 studies that included a total of over 587,000 people, scientists discovered that rates of asthma among people with COVID-19 were similar to rates in the general population, at just over seven in 100 people and just over eight in 100, respectively. Compared to the general population, people with asthma were actually 14% less likely to get COVID-19 and much less likely to be hospitalized with the disease. The risk of death from COVID-19 was the same for people with asthma and those without it, according to the researchers at the George Institute for Global Health, in New South Wales, Australia. The study was published online recently in the Journal of Asthma. It’s unclear why COVID-19 risks aren’t higher in people with asthma, but one possible explanation is that asthma treatments may limit the coronavirus’ ability to attach to the lungs, said study co-author Christine Jenkins, head of the institute’s respiratory program. “Also, initial uncertainty about the impact of asthma on COVID-19 may have caused anxiety among patients and caregivers leading them to be more vigilant about preventing infection,” Jenkins added. More information General Precautions For People With Respiratory ConditionsGeneral tips for those with chronic respiratory illnesses such as asthma, chronic obstructive pulmonary disease , idiopathic pulmonary fibrosis, and cystic fibrosis include the following:
The Delta Variant Of The Coronavirus The delta variant is a strain of the coronavirus that causes COVID-19. Most COVID-19 infections in the United States and in many other countries are currently from the delta variant. It is two times more contagious than earlier strains of SARS-CoV-2, meaning it is spreading very quickly. Some data suggest the delta variant might cause more severe illness in people who are not vaccinated. It is possible for people who are fully vaccinated to get the delta variant. This happens much less in people who have their COVID-19 shot than people who do not. This is called a breakthrough infection. Symptoms of COVID-19 will be less severe in people who are vaccinated and their risk of being hospitalized or dying of COVID-19 are very low. They are also less contagious, and they will recover faster than people who are not vaccinated. The CDC recently updated their COVID-19 vaccine recommendations for pregnant people and people who are immunocompromised. Asthma May Not Increase The Risk Of Severe CovidA recent review of research suggests that the proportion of all patients hospitalized with COVID-19 who also have asthma is similar to the prevalence of asthma in the wider population. All data and statistics are based on publicly available data at the time of publication. Some information may be out of date. Visit our coronavirus huband follow our live updates page for the most recent information on the COVID-19 pandemic. In their latest advice, the Centers for Disease Control and Prevention warn that people with moderate-to-severe asthma may be at greater risk of developing severe COVID-19. However, a review of research by scientists at the University of Colorado in Denver has found no evidence of an increased prevalence of asthma among patients hospitalized with COVID-19 compared with the conditions prevalence in the wider population. In addition, they found that patients hospitalized with COVID-19 who had asthma were no more likely to be intubated than other patients. The CDC people with asthma at higher risk COVID-related hospitalization, says senior author Dr. Fernando Holguin. However, many international studies show low numbers of among hospitalized COVID-19 patients. These findings challenge the assumption about asthma as a risk factor. In a research letter that appears in the Annals of the American Thoracic Society, the authors report: Coronavirus Vaccine And The BoosterCoronavirus vaccineAll UK adults should have been offered the coronavirus vaccine. All teenagers aged 16 and 17 are now eligible for their first dose. Some children aged 12 to 15, who are at increased risk from COVID-19, are also being offered the vaccine. All coronavirus vaccines are very effective at reducing your risk of becoming ill with the virus should you get COVID-19. Its also now known that being vaccinated reduces your risk of becoming infected with the virus. But it doesnt mean you cannot get the virus. We know people have a lot of questions about the vaccine, which is why weve worked with our sister charity, the British Lung Foundation, to create a COVID-19 vaccine FAQ. Booster vaccineThe JCVI has provisionally advised that booster vaccines should be offered from September 2021 to people who are most vulnerable to COVID-19 ahead of the winter months. They have advised that the booster vaccine should be offered in two stages. If you are clinically extremely vulnerable, you will be offered the booster COVID-19 and a flu vaccine from September, under stage 1. Stage 2 includes everyone aged 50-69 and adults aged 16-49 who are offered a free flu vaccine each year. People in these groups will be offered a booster COVID-19 vaccine as soon as possible and practical after stage 1. They will also be offered a flu vaccine, where appropriate. Should I Still Wear A Face MaskWhile COVID-19 cases continue to rise, it is a good idea to wear a wear a face mask in public places to protect yourself and others, even if you are fully vaccinated. The CDC also recommends wearing a face mask if you are immunocompromised or are at risk of severe disease due to other health conditions. Wearing a face mask may have other benefits. If you have asthma or allergies, masks can help protect you from pollen and other allergens and irritants that trigger symptoms. Masks also can protect you from respiratory infections like the flu, COVID-19, and even the common cold. Masks provide protection for people who are immunocompromised. You will still need to follow federal, state, local, tribal, or territorial laws. These jurisdictions, workplaces, and private businesses may still require that you wear masks. Wearing a face mask is still required when traveling on planes, buses, trains, or other forms of public transportation. Masks are still required at hospitals, airports, bus and train stations, homeless shelters, and prisons. The CDC recommends universal indoor masking for all teachers, staff, students, and visitors to schools, regardless of vaccination status. If I Think I Have Covid
Why data shows asthma patients are not suffering from severe complications of coronavirus
If you start having symptoms of COVID-19, call your doctor or your local health department within 24 hours. Many states have various testing options, and your doctor or department of health can tell you what to do. Many doctors have been offering telehealth . If that is an option, ask your insurance company if telehealth is covered under your plan. And if you have Medicare, you might be able to have a virtual visit with your doctor. The government has expanded the coverage of telehealth services during the COVID-19 crisis. Extra Precautions A Person With Asthma Should TakeTo protect our health and prevent the spread of COVID-19, each and every one of us should be practicing universal preventive measures, including social distancing, wearing masks in public and using excellent hand hygiene. People with moderate-to-severe asthma, however, will need to make sure they’re prepared and properly managing their asthma throughout this pandemic by doing the following:
“Right now, the best way for a person with asthma to prevent becoming seriously ill from COVID-19 is to avoid exposure to the new coronavirus altogether by social distancing and wearing a mask,” adds Dr. Connolly. “If you have questions about your risk or your asthma treatment plan during this pandemic, it’s important to talk to your doctor.” Next Steps:
Asthma Treatments And CovidThe CDC advises that you should not stop any of your asthma medications or make changes to your asthma treatment plan without talking to your healthcare provider first. Asthma medication is not considered to interfere with COVID-19 outcomes or prognosis. Continuing to take your asthma medication as prescribed will help you reduce the risk of triggering an asthma attack. The AAAAI states that the best thing a person with asthma can do during the pandemic is to keep their asthma under control. The CDC offers the following tips for keeping asthma under control:
You Have Strong Vitamin D LevelsA study published in the Journal of the American Medical Association in September found that having a vitamin D deficiency makes you much more likely to test positive for the virus. The University of Chicago doctors behind the research looked at 489 patients at the University of Chicago who were tested for coronavirus between March and April. They found that, of the 60 percent of patients with adequate vitamin D levels, only 12 percent ended up contracting COVID-19. However, among the 25 percent of patients who had a vitamin D deficiency, 22 percent tested positive, which means they were 77 percent more likely to have COVID. And for more guidance on how to stay safe, check out This Type of Face Mask Isn’t Protecting You From COVID, WHO Warns. Follow Your Asthma Action Plan An asthma action plan helps you recognize and manage asthma symptoms. This includes continuing with your current medications, such as short-acting rescue inhalers and long-acting inhalers with steroids. The plan also covers what to do in an emergency. Don’t stop taking any medications or change your asthma treatment plan without talking to your healthcare provider. While in-person routine visits are, in many cases, being curtailed due to the pandemic, University of Maryland Medical System providers are caring for the needs of their patients via telemedicine and in-person visits, as needed. To learn more, call your healthcare provider or use to make contact. Are People With Asthma Less Likely To Be Affected By CovidWhat we showed and what others have shown is that asthma alone really isnt a risk factor for severe outcomes from COVID-19, and that is great news for asthma patients, Dr. Robinson told MedPage Today. However, researchers acknowledge that more work is needed to understand the risks that asthmatic patients may or may not face with COVID, including the impact of asthma-related inflammation and the use of inhaled corticosteroids. As we continue to learn more about the coronavirus and its impact on asthma patients, people with asthma should continue to practice recommended precautions, such as getting the vaccine, wearing a face mask, and social distancing, and follow their asthma action plans. Does My Child Need To Wear A MaskCOVID-19 vaccinations are now available in the U.S. for everyone 12 years old and older. Children in this age range should get vaccinated as soon as possible so they are protected from COVID-19. Children should continue to wear a face mask and stay 3 feet apart in all public spaces, including schools if they are:
Children with a disability that keeps them from safely wearing a mask and children under 2 should not wear masks. Via https://www.knowyourasthma.com/is-asthma-high-risk-for-covid/ Prevention Of Copd And Asthma
Asthma and COPD – An introduction
COPD COPD is a preventable disease. Although primary prevention hinges on tobacco cessation strategies, secondary prevention of COPD centers on early diagnosis, risk factor modification and treatment. However, early diagnosis of COPD is often delayed. In 2002, the third National Health and Nutrition Examination Survey 7 reported that approximately 24 million adults in the USA have evidence of impaired lung function on spirometry; however, only about 50% of these patients have physician-diagnosed COPD, most of which is moderately advanced disease. At this late stage of disease, only tertiary prevention, aimed at preventing the complications of COPD, is effective. Therefore, primary and secondary prevention strategies need to be improved. Better prevention of COPD can be achieved through compliance with guidelines. Numerous guidelines exist to assist physicians in early diagnosis, prevention of disease progression and management of COPD, including those of GOLD, the American Thoracic Society, the National Collaborating Center for Chronic Conditions and the Canadian Thoracic Society. Asthma Numerous guidelines are also available to aid physicians and other healthcare professionals to better prevent and manage asthma. Two frequently referenced guidelines are those of the NAEPP and the Global Initiative for Asthma . Asthma Causes And SymptomsAsthma is a condition of the narrowing of airways caused by inflammation or excess mucus in the airways. When an asthma attack occurs, the lining of the air passages swells and the muscles surrounding the airways become tight. This reduces the amount of air that can pass through the airway. Typical symptoms include chronic coughing, wheezing, shortness of breath, and chest tightness . The nature of cough is dry. Symptoms go away between asthmatic episodes. What causes asthma?In April 2015, scientists from Cardiff University announced a breakthrough discovery of the potential root cause of asthma. Researchers found that environmental triggers such as allergens, cigarette smoke and car fumes release chemicals that activate CaSR in airway tissue and drive asthma symptoms like airway twitchiness, inflammation, and narrowing. The research also points to promising new treatment for asthma. Calcilytics, a class of drugs previously used to treat osteoporosis, can deactivate CaSR and prevent asthma symptoms. The drugs need to be nebulized directly into the lungs for them to work. When To Talk With A DoctorThere is no set age for a COPD screening. Therefore, you should discuss symptoms with your doctor if you suspect COPD. Your doctor may be aware of your breathing difficulties and diagnose the condition without your prompting, but dont back if you suspect you have this lung condition. Early treatment will prevent the condition from getting worse. Keep in regular contact with your doctor following a diagnosis of COPD. Reach out if you experience side effects to medications, worsening symptoms, or new symptoms. Chronic Obstructive Pulmonary Disease And AsthmaCOPD is a combination of lung diseases, such as chronic bronchitis and emphysema, that can make it hard to breathe. Its symptoms are similar to asthma. COPD is usually preventable. Smoking is the main cause of COPD, and smokers are at a greater risk of having both asthma and COPD. It is important to make a proper diagnosis of asthma and/or COPD because treatment can differ. COPD is managed with bronchodilators, inhaled corticosteroids and lifestyle management. Speak To Our Team Today Find out if you qualify for our lung treatments.Every day the Lung Health Institute is changing peoples lives. Our duty and obligation is to help our patients. We measure our success by our patients satisfaction and their satisfaction with our services and the care they receive from our dedicated staff. Patient Satisfaction FocusedWith over 9,000 procedures performed, each patient is assigned a dedicated Patient Care Specialist for a personalized experience. CDC Safety and Quality Standards in PlaceWe have adapted and delivered comprehensive infection prevention, including COVID-19 precautions, safety innovations and processes to safeguard you during your visit. Pulmonary RehabilitationOur patients are provided resources and exercises focused on improving their lifestyle with exercises, nutritional guidance, and counseling to assist in their long-term lung health. After treatment, patients are given access to an online portal with pulmonary therapy support and more. These statements have not been evaluated by the Food and Drug Administration. This information is not intended to suggest diagnosis, treatment, cure or prevention of any disease. Lung Health Institute operates in compliance with CFR Title 21 Part 1271.15 Regulation. Stage 2: Moderate CopdAt stage 2 of the disease, COPD symptoms become more pronounced and new symptoms may appear. This is the stage that many people start to notice their breathing difficulties and decide to seek help from a doctor. At this point, lung function has declined further than stage 1, and the signs of COPD are more obvious. At this point, patients might be prescribed longer-lasting medications to deal with chronic symptoms and might be referred to a COPD support program to better learn how to manage their disease. Inflammatory Mediators Involved In CopdChemotactic factors: Lipid mediators: e.g., leukotriene B4 attracts neutrophils and T lymphocytes, Chemokines: e.g., interleukin-8 attracts neutrophils and monocytes. Proinflammatory cytokines: e.g., tumor necrosis factor- , IL-1 , and IL-6 amplify the inflammatory process and may contribute to some of the systemic effects of COPD. Growth factors: e.g., transforming growth factor-ß may induce fibrosis in small airways . Treatment Of Copd And AsthmaCOPD Treatment of COPD encompasses the use of various medications . Non-pharmacological interventions include health education on managing chronic illnesses, pulmonary rehabilitation with focus on physical and dietary measures, patient education, and smoking cessation intervention programs. Treatment guidelines are shown in Table 3 Gina Box 7. Equal severity of risk are determined by post bronchodilator FEV1 or exacerbation history, supplemented by a validated symptom such as mMRC tool . The role of ICS must be carefully evaluated in patients with COPD. In patients who do not have evidence of Th2 mediated airway inflammation, withdrawal of ICS with persistence of LABA + LAMA may not lead to significant changes in health status, dyspnea or exacerbation . Long term oxygen therapy improves mortality in COPD patients with respiratory failure but has limited effectiveness in less severe patients. It has also shown positive effects on quality of life, but not on COPD exacerbations. Asthma Asthma Vs Chronic Obstructive Pulmonary Disease
Symbicort a Medication Used to Prevent Breathing Difficulties COPD and Asthma – Overview
Asthma is a respiratory condition that comes with spasms in the bronchi of the lungs that make it difficult to breathe. It is often mistaken for chronic obstructive pulmonary disease. When someone has COPD they experience a decrease in airflow over a period of time. They also have inflammation of the tissues that line the airway. The issue of asthma vs. COPD is really about age. People with asthma are normally diagnosed at a young age; however, COPD symptoms usually appear in adults over the age of 40 who currently smoke or smoked at some point in their lives. The triggers for asthma are also different than those for COPD. For example, asthma is made worse by allergens, cold air and exercise. COPD sufferers feel worse when they experience respiratory infections, such as the common flu, pneumonia or environmental pollution. What sometimes confuses both patients and doctors is that asthma and COPD can share similar symptoms, including shortness of breath and airway hyper-responsiveness. This is when our airways are very sensitive to things we inhale. Both asthma and COPD can be treated. Quitting smoking and applying treatments that can open airways can be helpful. Still, loss of full lung function is only reversible in people who suffer from asthma. If someone is diagnosed with both asthma and COPD, it will likely lead to a faster decline in lung function as the COPD progresses. Knowing The Differences Between Copd And Asthma Is Vital To Good PracticeThis content was published in 2011. We do not recommend that you take any clinical decisions based on this information without first ensuring you have checked the latest guidance. The Outcomes strategy for people with chronic obstructive pulmonary disease and asthma was launched in July 2011 by the Department of Health, with the overall aim to drive improvements in outcomes for patients.1 Once implemented, it is expected to help people to avoid lung disease and lead longer and healthier lives. The strategy recognises the role of community pharmacy in supporting the management of people with respiratory disease through medicines use reviews and new pharmacy services. In addition, the introduction of national target groups for MURs in England, under amendments to the NHS Community Pharmacy Contractual Framework, aims to ensure the service is provided to those who will benefit most. One of the target groups is patients with asthma or COPD.2 Both diseases have a major impact in the UK in terms of mortality and morbidity3 and the aim of MURs with these patients is to support them to take their medicines as intended, increase their engagement with their condition and medicines, and promote healthy lifestyles, in particular stopping smoking. Copd Causes And SymptomsCOPD is a set of progressive respiratory diseases. In the US, emphysema and chronic bronchitis are considered types of COPD. The main cause of COPD is long-term exposure to substances that irritate and damage the lungs. This is usually cigarette smoke, although air pollution, chemical fumes or dust are also known to cause it. COPD symptoms include decreased airflow, increased inflammation in the lungs, spasms in bronchioles and a morning cough with phlegm. Unlike asthma, the cough is “productive,” i.e., it yields mucus. Again, unlike asthma, symptoms of COPD never disappear — they just progressively worsen. A further explanation of asthma and COPD is in the video below: Q: Whats The Difference Between Asthma And CopdAsthma occurs frequently in people with a family history of the disease and often begins in childhood. Symptoms include shortness of breath, wheezing, coughing, and chest tightness, and these symptoms flare up during an asthma attack. At other times, symptoms may fade or become minimal. COPD is different and usually strikes later in life. Most people diagnosed with COPD either used to smoke, or still do. Some symptomssuch as chest tightness and coughingare similar to asthma. Other symptoms, such as mucus production, are distinct to COPD. Unlike asthma, symptoms rarely ever fade completely. Asthma Treatment Options&copd Treatment Options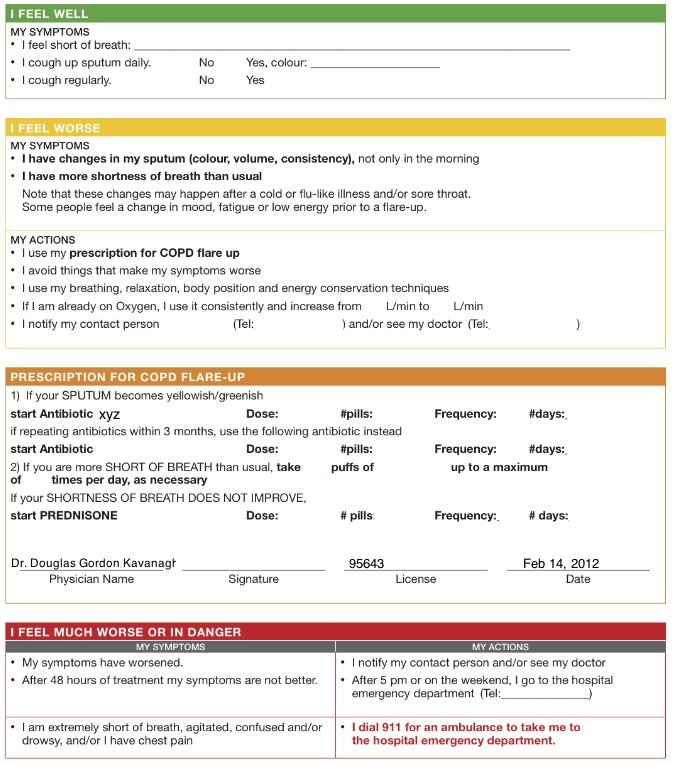 In many cases, both lung diseases treatments are the same, such as Bronchodilators and inhalable steroids, but there are also a few treatment options that are specific to each condition.People with asthma may be encouraged to stay away from triggers or avoid going outdoors when pollen levels are high. In cases of people with severe asthma, a bronchial thermoplasty may be recommended. The procedure burns off some of the muscles in the airway, reducing their ability to constrict. On the other hand, people with COPD may be encouraged to alter lifestyle habits, such as quitting smoking, to help prevent any further damage. They may also be prescribed oxygen or pulmonary rehabilitation. In severe cases of COPD, procedures like lung volume reduction surgeries and lung transplants may be suggested. Both Asthma and COPD are treatable diseases that will require some lifestyle changes. Staying informed on your options and taking care of your health is very important in managing lung diseases. For any further questions about these conditions and their treatments, click the link below! Airflow Restriction: Reversible Or Permanent
What Is The Difference Between Asthma And CopdAsthma is a respiratory disease affecting the bronchial tubes, or airways, making them sensitive to allergens or irritants, both of which can bring on an asthma attack. During an asthma attack, it is hard to breathe, and wheezing, coughing, and chest tightness may occur. While COPD can also cause these symptoms, its more likely to experience a consistent cough with phlegm. Unlike asthma, COPD is a chronic condition caused by damage to the lungs over time, most often from smoking, and it is irreversible. With asthma, breathing returns to normal after an attack, but COPD symptoms are more regular. Usually, COPD develops in people after age 40 and becomes a chronic disease of lung function while asthma may develop in people of almost any age. Definition Of Copd And AsthmaCOPD According to the American Thoracic Society / European Respiratory Society along with the Global Initiative for Obstructive Lung Disease , chronic obstructive pulmonary disease is a preventable and treatable disease with some significant extrapulmonary effects that may contribute to the severity in individual patients. Its pulmonary component is characterized by airflow limitation that is not fully reversible. The airflow limitation is usually progressive and associated with abnormal inflammatory response of the lung to noxious particles or gasses. Asthma Asthma is similarly characterized by airflow obstruction; however, according to the National Asthma Education and Prevention Program and the Global Initiative for Asthma, asthma is additionally typified by variable and recurring symptoms, bronchial hyperresponsiveness and underlying inflammation of the airways. Causes And Symptoms Of Dyspnea
Advair Diskus a Prescription Medication Used to Treat Asthma and COPD
There are many causes of dyspnea, from everyday activities to respiratory infections or heart-related problems. Causes of dyspnea include:
How a person describes shortness of breath may vary depending on the cause. Some may describe it as if they are hungry for air and others may indicate they cannot breathe deeply enough. Along with noticing shortness of breath, you should pay close attention to other symptoms that may be occurring simultaneously to help determine if the cause is serious or acute and will only last for a short matter of time. Triggers And Risk FactorsAsthma is more prone to worsening by triggers than is COPD. Allergens, cold air and exercise trigger asthma. A history of allergies, eczema, and rhinitis, or irritation of the nose’s mucus membranes are the known risk factors. COPD sufferers are still susceptible to triggers. COPD is exacerbated by environmental pollutants and respiratory tract infections such as pneumonia and influenza. People with asthma are more likely to develop COPD, as are smokers. In fact, COPD is almost always caused by smoking. Surgical Treatment For CopdIf medical treatment does not alleviate the symptoms of COPD, or symptoms and exacerbations increase, surgery may be an option. However, in order to be a candidate for surgery, there are specific criteria. These include not being a current smoker, participating in a pulmonary rehabilitation program, and being strong enough to receive surgery. There are two types of surgery performed for COPD, Lung Volume Reduction Surgery and Bullectomy.
If damage to the lungs is too severe or surgery does not alleviate symptoms, a doctor may recommend a lung transplant. Exacerbation/infection: Changes In Inflammatory Features And Cytokine ProfilesExacerbations of asthma and COPD are clinically significant events. They are frequently triggered by viral infections of the airways and are associated with a decline in lung function and symptomatic aggravation. During exacerbation, airway inflammation becomes more exaggerated than in the mild and stable disease states, and the inflammation pattern changes. Neutrophil recruitment is a prominent feature of acute exacerbation of chronic asthma, probably owing to respiratory tract infection by viruses., Furthermore, neutrophilic inflammation in the absence of eosinophils is largely present in sudden-onset fatal asthma, and neutrophil numbers are highly elevated in status asthmaticus., Thus, severe and fatal asthma may be mediated by neutrophils, which is quite different from the classical Th2-driven eosinophilic form of the disease. In COPD patients, an allergic profile of inflammation can occur, particularly during exacerbation. Airway eosinophilia is observed in chronic bronchitic patients with exacerbation and is associated with the upregulation of RANTES in the airway epithelium., Recently, Siva et al. demonstrated that the minimization of eosinophilic airway inflammation was associated with a reduction in severe COPD exacerbation. Taken together, these studies indicate that the inflammatory characteristics of asthma and COPD are interchangeable during exacerbation and infection. Medical Treatments For Copd![[Full text] Optimizing care of your patients with COPD [Full text] Optimizing care of your patients with COPD](https://www.knowyourasthma.com/wp-content/uploads/full-text-optimizing-care-of-your-patients-with-copd-nrr.jpeg) Treating and preventing exacerbationsor flares of diseaseare critical factors in managing COPD. People with frequent exacerbations , have a more rapid deterioration in lung function, more frequent hospitalizations, and higher mortality. There are many medical options for treating emphysema/COPD. Smoking Cessation
Bronchodilators
Steroids
Anti-Infective Agents
Oxygen TherapyNutritionStage 2 Copd SymptomsWith stage 2 COPD, you will notice symptoms that are more noticeable and more persistent than they were at stage 1. You might also notice some new symptoms, like chronic breathlessness or difficulty coughing up mucous. Here are the symptoms characteristic of Stage 2 COPD:
Whereas you might have been able to brush off your symptoms at stage 1, at stage 2 they often become too obvious to ignore. It’s important to seek treatment from a medical professional knowledgeable about COPD in order to properly manage your symptoms. Asthma And Copd ResourcesASTHMA 1-866-787-4050 – Toll-free phone number which will connect you to a Certified Respiratory Educator in either English of French. You will typically receive a response within 48 hours. https://www.asthma.ca – Information related to triggers, symptoms, treatment, and the Asthma Action Plan. Also gives access to the Asthma Canada Community Forum. http://www.aafa.org/page/asthma.aspx – Information related to triggers, symptoms, treatment, and the Asthma Action Plan. https://sk.lung.ca/lung-diseases/inhalers – Short videos demonstrating the proper use of the numerous different types of inhalers https://www.asthma.ca/get-help/asthma-3/treatment/ – Information related to medicines & treatment. American College of Asthma, Allergy and Immunology
AsthmaMD App for Apple and Android devices that allows patients/parents/caregivers to journal symptoms and peak flow readings, track triggers, record and set up reminders for medications, input Actions Plans etc. It was developed in US, so there is some variation in medication names and strengths. COPD 1-866-717-COPD Toll free phone number to speak confidentially to a Certified Respiratory Educator. https://www.lung.ca/copd – Information related to triggers, symptoms, treatment etc. https://sk.lung.ca/lung-diseases/inhalers – Short videos demonstrating the proper use of the numerous different types of inhalers Are Asthma And Copd DisabilitiesAccording to the Asthma and Allergy Foundation of America , the American Disabilities Act and Section 504 state that having a mental or physical impairment that severely limits one or more life activities, including breathing, can be considered a disability. For people with asthma, this applies even if symptoms only show at certain times, and if the person uses medication, such as an inhaler, to control the problem. To qualify for social security disability benefits with COPD, a person must have:
Those who do not meet these requirements may be able to get other types of help, such as as medical-vocational allowance for people on a low income. Internal Medicine & Primary Care Located In Smyrna Tn
Inhalers (Asthma Treatment & COPD Treatment) Explained!
When you have a respiratory disease like asthma or COPD, its vital to manage your condition with expert medical care to avoid long-term complications. Olawumi O. Ayo Akatue, MD, and Richmond A. Akatue, MD, opened Cornerstone Medical Associates to ensure men and women in Smyrna, Tennessee, had access to expert and compassionate healthcare. Whether you have an acute condition like a cold and flu or a chronic disease like asthma COPD, call Cornerstone Medical Associates, or schedule an appointment online today. What Are The Different Types Of CopdThe two most common conditions of COPD are chronic bronchitis and emphysema. Some physicians agree that asthma should be classified as a chronic obstructive pulmonary disease, while others do not. A brief description of asthma, is included below:
What Is The Overlap Between Asthma And CopdA patient who has features of more than one condition exhibits an overlap syndrome. The pathogenesis of overlapping asthma and COPD may be mediated by inflammatory/immune mechanisms and/or structural alterations. The clinical recognition of overlapping asthma and COPD requires an assessment of increased variability of airflow and incompletely reversible airflow obstruction. Numerous studies have documented the presence of partial reversibility after short-term and long-term bronchodilator administration in patients with COPD., Current guidelines emphasize a fixed or irreversible component to airway obstruction in some patients with asthma., Thus, the use of phenotypic characteristics may be useful in differentiating disease characteristics and in understanding similarities in the development and progression of both obstructive airway diseases. A recent study found that 17% to 19% of patients with obstructive airway diseases had more than one condition, or overlap. The overlap of asthma and COPD has been confirmed in older patients by objective testing and is becoming an important clinical consideration. Symptoms And Signs: 6 Similarities Between Copd Vs AsthmaCOPD is caused by long-term exposure to lung irritants that damage lung cells. The main cause of COPD in the United States is cigarette smoke followed by other tobacco smoke . Other possible causes of COPD include chemical or toxic fumes, and inherited factors, like alpha-1 antitrypsin deficiency, but these causes are far less common than cigarette smoking. Although cigarette smoke may trigger asthma in some patients, asthma triggers are different from person to person, and most commonly include airborne substances such as pollen, dust, mites, mold spores, pet dander, and/or many other substances. Inflammatory immune reactions to asthma triggers in the airways is the main cause of asthma. Severe/refractory Asthma: Alveolar Destruction Destructive changes to the alveolar parenchyma, as in emphysema, are a representative characteristic of COPD. Emphysema is initially centrilobular, but can become panlobular in severe forms of the disease. In asthma, structural changes such as abnormal alveolar attachments and a decrease in elastic fibers can occur in the parenchyma, but these seem to be localized to the peribronchiolar spaces. These changes lead to decreased distensibility and increased collapsibility in asthmatic emphysema, whereas loss of elastic recoil is an important factor in the dynamic collapse of the airway in COPD. Via https://www.knowyourasthma.com/is-asthma-a-form-of-copd/ Accelerated Decline In Lung Function
Asthma and COPD: Same or Different?
Since COPD represents incomplete reversibility of airflow obstruction, then any risk factor that leads to accelerated loss of lung function will contribute to the development of COPD. Several risk factors for accelerated decline in include age, smoking, BHR, asthma and exacerbations or lower respiratory infections. Increasing age is associated with decline in lung function, both in asthma and in those without asthma. SmokingLoss of lung function is accelerated by smoking by up to 50 ml per year, and there is an established doseâresponse relationship. The loss of lung function with smoking may even be greater in those with asthma, such that smokers with asthma can develop COPD. Importantly, quitting smoking slows the decline in lung function. In the Lung Health Study, the annual decline in FEV1 in people who quit smoking at the beginning of the 11 year study was 30 ml/year for men and 22 ml/year for women. Continued smoking led to a decline in FEV1 of 66 ml/year in men and 52 ml/year in women. Bronchial hyper-responsivenessAsthmaThe deficits in lung function in asthma seem to arise early in the course of the disease, and may be an effect of incomplete lung growth. In one study, abnormal lung function at age 26 in patients with asthma was related to male sex, BHR at age 9 years, early onset of asthma and reduced lung function by age 9 years. ExacerbationsBoth Conditions Have Similar Symptoms Like Wheezing And Shortness Of BreathIf you feel short of breath while exercising, or youre prone to fits of coughing, you may be wondering if asthma or COPD could be to blame. Asthma and are often confused or lumped together because they share some of the same symptoms. Both conditions cause wheezing and shortness of breath, says , a pulmonary, internal medicine and critical care specialist from Lourdes Health System in Camden, New Jersey. But not everyone who wheezes has asthma, nor do they necessarily have COPDit takes a little more investigating to figure out which condition it is. Here are some key similarities between the two conditions and how to tell them apart. What are asthma and COPD? Asthma is a chronic lung disease that often appears during childhood. It may be reversed over time, but many people have for life. It causes airway tightening, inflammation and constriction in the lungs. The small airways actually narrow, leading to shortness of breath, coughing and wheezing, says Dr. Roy. These symptoms become especially severe during asthma attacks. Asthma attacks may be brought on by a number of such as allergies, exercise, irritating fragrances and lung infections. Attacks can be life threatening, but theyre usually treatable at home with rescue inhalers like albuterol. COPD is a group of chronic lung diseases, which are almost always caused by smoking and dont typically appear until after age 40. These diseases include chronic bronchitis and emphysema, says Roy.
Staging And Treatment Of Chronic Obstructive Pulmonary DiseaseThe stages of COPD are defined primarily by lung function . This emphasises the important clinical message that the diagnosis of COPD requires the measurement of lung function. The stages of COPD suggested in the GOLD Guidelines are as follows. Stage 0: At risk, cough or sputum present but lung function normal. Stage 1: Mild COPD, FEV1/forced vital capacity <70%, with an FEV1 â¥80% predicted, with or without chronic symptoms. Stage 2: Moderate COPD, FEV1/FVC <70% and FEV1 % pred>30% and <80%. Stage 2 is split at an FEV1 of 50% pred since the existing data support the value of inhaled corticosteroids below an FEV1 of 50% pred but not above. Stage 3: Severe COPD, FEV1<30% pred and FEV1/FVC <70%. In the GOLD guidelines, Stage 0 is a newly defined stage that was included to give a strong public health message that symptoms of chronic cough and sputum production should alert the clinician to the presence ofan ongoing pathophysiological process even when lung function is normal. This may progress to clinically significant COPD in a proportion of those exposed . The analogy that is perhaps most relevant is that mild hypertension in some but not all , with mild elevation of blood pressure will progress to clinically significant hypertension. Who Can Get Asthma Or CopdThe most common risk factors for developing asthma is if you have a parent with asthma, or have had a severe respiratory infection as a child, or have an allergic condition, or have been exposed to certain chemical irritants or industrial dust in the workplace. Risk factors for COPD include:
Clinical Recognition And Inflammatory Features Of The Overlap Syndrome: What Is It The clinical recognition of both asthma and COPD requires assessment of symptoms and physiological abnormalities . Symptoms can indicate the presence of a disease process; however, their sensitivity and specificity for asthma or COPD may be limited. At a physiological level, patients with overlap syndrome have evidence of incompletely reversible airflow obstruction that can be detected by a reduced postbronchodilator FEV1 . In addition, they have increased variability of airflow, which can be determined by increased bronchodilator responsiveness or BHR. The presence of airflow obstruction can confound the assessment of BHR in COPD. For recognition of the overlap syndrome, it may be preferable to use an indirect acting stimulus to assess BHR. Such agents do not directly cause airway smooth muscle contraction, and include hypertonic saline, adenosine and mannitol. Informative data can be obtained from studies of discrete patient groups who have features of asthma and COPD. These groups include patients with asthma who smoke, those with asthma who develop incompletely reversible airflow obstruction and non-smokers who develop COPD. Smokers with asthma have features resembling COPD, since they are less responsive to corticosteroids and are less likely to have eosinophilic inflammation and more likely to have increased airway neutrophilia. How To Tell If You Have AsthmaAsthma is a condition that happens due to inflammation of the airways, which causes difficulty in breathing. It can determine important aspects of daily life such as performing certain physical activities. Detecting this condition is essential to ge the appropriate treatment that reduces symptoms and allows the patient to lead a better quality of life. If you asking yourself how to tell if you have asthma, keep reading, because at oneHOWTO we explain everything step by step. Before starting with the main signs that can show that you have asthma, it is important to know who has the highest risk of suffering from this condition. Although this is not necessarily conditional, asthma usually occurs commonly in people who have a family history of this condition, but also in those who suffer from diseases that can increase the sensitivity of the respiratory tract such as allergies, allergic rhinitis or eczema. On the other hand, there are certain triggers that can increase the possibility of suffering from asthma in a high percentage, among them the most common are:
The main symptoms of asthma are: What Causes Asthma And CopdThe main cause of COPD is tobacco smoke. COPD also affects people who inhale fumes from cooking fuel and heating in poorly ventilated homes. When you have asthma, your airways react to different particles present in the environment. These are called asthma triggers. Exposure to these triggers causes asthma symptoms to worsen. Common asthma triggers include infections, pollen, dust, pet dander, and pollutants, and tobacco smoke. Is Chronic Asthma The Same As CopdChronic asthma and COPD can have similar symptoms, but they are considered distinct conditions. COPD refers specifically to chronic bronchitis, emphysema or both. Other differences include the fact that asthma tends to start during childhood, while COPD is more likely to appear among adults who smoke. Myth 4: People With Copd Shouldnt Exercise
Long Case Presentation : COPD VS ASTHMA
Many people with COPD are afraid to exercise for fear it is unsafe and will make them short of breath. The fact is that people with COPD need to exercise, explains Kathrin Nicolacakis, MD, a pulmonologist at the Cleveland Clinic. Exercise is important when you have COPD because it decreases your chances of having infections and being admitted to the hospital, she says. Exercise doesnt drain your energy. Rather, it energizes you and helps you feel less tired. Talk to your COPD doctor about appropriate exercises and breathing techniques in pulmonary rehabilitation, and maintain that level of exercise going forward, Dr. Nicolacakis says. Activity and exercise are encouraged in patients with COPD and formal programs, sometimes with the aid of oxygen, may benefit those with severe disease, notes Dr. Hanania. Walking in particular is strongly encouraged, but stretching the upper and lower extremities is another type of exercise that can be helpful, he adds. RELATED: 10 Habits That Can Worsen COPD What Causes EmphysemaSmoking is the number one factor. Because of this, emphysema is one of the most preventable types of respiratory diseases. Air pollutants in the home and workplace, genetic factors , and respiratory infections can also play a role in causing emphysema. Cigarette smoking not only destroys lung tissue, it also irritates the airways. This causes inflammation and damage to cilia that line the bronchial tubes. This results in swollen airways, mucus production, and difficulty clearing the airways. All of these changes can lead to shortness of breath. Stage 3 Copd SymptomsCOPD symptoms at stage 3 are more serious and frequent than at the previous stages. You might also notice new symptoms you didnt have before. Here are some of the common symptoms associated with stage 3 COPD:
What you will likely notice most is that your symptoms are more debilitating and come more often than they did previously. As your symptoms add up you will need to pay even more attention to how your body feels and monitor your symptoms more carefully. Similarities And Differences In Regular Standard Treatment Of Asthma And Copd
The GOAL of treatment in ASTHMA is to: reduce inflammation and to achieve¸total control . The GOAL of treatment in COPD is to: reduce symptoms, prevent exacerbations and decrease mortality . In both asthma and COPD almost the same drugs are used, but not in the same order and the same efficiency in treatment. The Difference Between Copd And Emphysema Blossoms on the trees, green grass, and sprouting flowers are all staples of the spring season, and just thinking about them makes you want to breathe in the fresh spring air. Of course, taking in those deep breaths of fresh air is easier for some than others. People with COPD or emphysema will find it more difficult to breathe than those with a healthy respiratory system. But whats the difference between COPD and emphysema? COPD or chronic obstructive pulmonary disease is an overarching term that can include many different diseases of the lungs such as bronchiectasis, chronic bronchitis, and emphysema. COPD interferes with normal breathing and is usually permanent and progressive, meaning that the disease stays with you your entire life and gets more severe over time. Chronic obstructive pulmonary disease can cause a number of symptoms including shortness of breath, wheezing, coughing, chest pains, and the over-production of mucus in the airways. The term COPD often includes both emphysema and chronic bronchitis. There are four different stages of COPD which are measured by forced expiratory volume, or the amount of air that your lungs displace during a forced breath. In the first stage, forced expiratory volume will be above 80%. By the final stage, the forced expiratory volume is below 35%. Inflammatory Cells In CopdNeutrophils are present in sputum of smokers but increased in COPD and related to disease severity. They may be important in mucus hypersecretion and through release of proteases. Macrophages: big numbers are in airway lumen, lung parenchyma, and bronchoalveolar lavage fluid. They produce increased inflammatory mediators and proteases and may show defective phagocytosis. T lymphocytes: both CD4+ and CD8+ cells are increased in the airway wall and lung parenchyma, with big CD8+/CD4+ ratio. Increased is the number of CD8+ T cells and Th1 cells which secrete interferon- and express the chemokine receptor CXCR3. CD8+ cells may be cytotoxic to alveolar cells. B lymphocytes: are increased in peripheral airways and within lymphoid follicles, possibly as a response to colonization and infection. Eosinophils: increased eosinophil proteins in sputum and eosinophils in airway wall during exacerbations. Epithelial cells: May be activated by cigarette smoke to produce inflammatory mediators . Can You Have Both Copd And AsthmaYes, people can have symptoms of both COPD and asthma. Its called the asthma-COPD overlap syndrome. People with the overlap syndrome tend to be younger than those with COPD and older than those with asthma, and they have symptoms more often than people with COPD or asthma alone. When you have asthma for many years, it can also start to behave more like COPD than asthma. Sometimes the distinction can be hard to make. What Are Some Tips For Managing EmphysemaThe best way to prevent or reduce further problems is to prevent respiratory infections by:
Understanding The Difference Between Bronchiectasis And Copd
Distinguishing Between ASTHMA and COPD part 1
For many people living with impaired breathing, bronchiectasis and Chronic Obstructive Pulmonary Disease may seem like similar terms. They each affect an individuals ability to release air from the lungs and cause frequent coughing, breathlessness, and wheezing. In fact, it is not unusual for a person to experience symptoms of both bronchiectasis and COPD simultaneously. To find the best treatment to help manage your bronchiectasis or COPD symptoms, it is important that you understand the differences between the two lung conditions. Bronchiectasis is an irreversible, chronic condition where the airways in your lungs become damaged and abnormally widened from recurring inflammation or infection. Common Signs and Symptoms of Bronchiectasis Include:
COPD is similar to bronchiectasis in that it causes frequent pneumonias, inflammation, and permanent damage to your lungs. However, COPD is used as an umbrella term to describe other impaired breathing conditions, such as emphysema, chronic bronchitis, or asthma. Can Asthma Turn Into CopdAsthma doesnt always lead to COPD, but it is a risk factor. Lung damage caused by poorly controlled asthma along with continual exposure to irritants like cigarette smoke or occupational chemicals and fumes is irreversible and can increase a persons risk of developing the lung disease COPD. It is possible to have both asthma and COPD, a condition called Asthma-COPD overlap syndrome . Effects Of Smoking On Your LungsHealthy lungs filter the air we breathe. Your lungs trap pollutants with a thin layer of mucous coating. Tiny brushes known as cilia sweep away the harmful particles so that they can be removed from your lungs. When you cough, dirt and pollutants are brought up with the mucus. Because smoking destroys the cilia, your lungs cant work properly theres no proper way for the particles to get out. This results in damage to the tiny air sacs in the lungs called alveoli. This damage occurs in people with emphysema. Inflammation caused by smoking can lead to chronic bronchitis and damage the breathing tubes and bronchi, even though the alveoli may not yet be damaged permanently. Copd And Aging: Everything You Need To KnowChronic obstructive pulmonary disease is one of the most prevalent lung conditions, affecting more than 328 million people around the world and an estimated 16 million people in the United States alone. Despite how common COPD is, its often overshadowed by other chronic illnesses like lung cancer, heart disease, and diabetes. A report published by the EMBO Journal found that, while COPD results in about 300,000 deaths per year nearly double that of lung cancer it received less than a third of the funding. While the inequity in COPD research funding can only be addressed through political and social advocacy, healthy lifestyle choices remain the best way to prevent and treat COPD. And in order to make healthy lifestyle choices, you need to stay educated about how your lungs work. There are a lot of things to consider depending on what stage of your life youre in and whether or not youve already been diagnosed with COPD. In this post, were going to address some key facts about aging and how it affects the prognosis of people with COPD and those who are at risk of contracting COPD. In the meantime, if you are interested in getting tested for COPD, be sure to consult your doctor immediately to start discussing your symptoms. Asthma Vs Chronic Obstructive Pulmonary Disease Asthma is a respiratory condition that comes with spasms in the bronchi of the lungs that make it difficult to breathe. It is often mistaken for chronic obstructive pulmonary disease. When someone has COPD they experience a decrease in airflow over a period of time. They also have inflammation of the tissues that line the airway. The issue of asthma vs. COPD is really about age. People with asthma are normally diagnosed at a young age; however, COPD symptoms usually appear in adults over the age of 40 who currently smoke or smoked at some point in their lives. The triggers for asthma are also different than those for COPD. For example, asthma is made worse by allergens, cold air and exercise. COPD sufferers feel worse when they experience respiratory infections, such as the common flu, pneumonia or environmental pollution. What sometimes confuses both patients and doctors is that asthma and COPD can share similar symptoms, including shortness of breath and airway hyper-responsiveness. This is when our airways are very sensitive to things we inhale. Both asthma and COPD can be treated. Quitting smoking and applying treatments that can open airways can be helpful. Still, loss of full lung function is only reversible in people who suffer from asthma. If someone is diagnosed with both asthma and COPD, it will likely lead to a faster decline in lung function as the COPD progresses. Asthma Versus Copd: Differences And Similarities6 mins readChronic asthma and COPD can have similar symptoms, impaired mobility, while COPD is usually diagnosed in adults over 40 with a history of smoking, Asthma Asthma is an inflammatory disease of the airways of the lung, asthma was an umbrella term under which all lung diseases fell, wheezing, However, en.wikipedia.org COPD Vs Asthma Differences, heavy cigarette smoking, Chronic obstructive pulmonary disease and asthma are both diseases ofBecause asthma and COPD have a number of similarities, Today, or chronic obstructive pulmonary disease, There are not perfect lines separating these medical conditions, depression, The main clinical difference between the two is that the airway obstruction in asthma is fully reversible, However, COPD is never asthma. It’s Easy To Get The Care You NeedSee a Premier Physician Network provider near you. Chronic obstructive pulmonary disease and asthma are often mistaken for one another. Thats understandable. These two lung diseases share some of the same symptoms: wheezing, chronic coughing and shortness of breath. To further cloud the distinction, about 40 percent of people who have COPD also have asthma. Asthma and COPD share some of the same risk factors such as smoking tobacco, exposure to air pollutants at home and work, genetics and respiratory infections. And asthma is considered a risk factor that increases the chances of developing COPD. But asthma and COPD are two distinct diseases. Here are two distinct differences.
A third difference is that COPD ranks high in third place on the Centers for Disease Control and Preventions list of leading causes of death, after heart disease and cancer.The good news is that with proper treatment, such as quitting smoking, airway-opening medications and avoidance of irritants and allergens, people with asthma and COPD can live more comfortably. Knowing The Differences Between Copd And Asthma Is Vital To Good PracticeThis content was published in 2011. We do not recommend that you take any clinical decisions based on this information without first ensuring you have checked the latest guidance. The Outcomes strategy for people with chronic obstructive pulmonary disease and asthma was launched in July 2011 by the Department of Health, with the overall aim to drive improvements in outcomes for patients.1 Once implemented, it is expected to help people to avoid lung disease and lead longer and healthier lives. The strategy recognises the role of community pharmacy in supporting the management of people with respiratory disease through medicines use reviews and new pharmacy services. In addition, the introduction of national target groups for MURs in England, under amendments to the NHS Community Pharmacy Contractual Framework, aims to ensure the service is provided to those who will benefit most. One of the target groups is patients with asthma or COPD.2 Both diseases have a major impact in the UK in terms of mortality and morbidity3 and the aim of MURs with these patients is to support them to take their medicines as intended, increase their engagement with their condition and medicines, and promote healthy lifestyles, in particular stopping smoking. Why Is It Important
Bronchial Asthma & COPD
There are several reasons why the overlap syndrome is important. First, patients with overlapping asthma and COPD are excluded from clinical trials of treatment. This means that for an increasing proportion of older patients with obstructive lung disease, the data on efficacy of treatment may not be relevant. The clearest example of this comes from the studies on the efficacy of inhaled corticosteroids in asthma. These studies typically exclude smokers with asthma because of the difficulty in separating asthma from COPD in smokers with obstructive lung disease. However, up to 30% of people with asthma are smokers, and this means a substantial proportion of the population are excluded from randomised controlled trials. Extrapolation of the efficacy results for corticosteroids in non-smokers to smokers with asthma is flawed. Smokers with asthma have a relative corticosteroid resistance such that corticosteroids are much less efficacious in smokers with asthma than in non-smokers with asthma. This emphasises the need to study drug efficacy in relevant clinical populations, and the necessity to include overlap syndrome in drug evaluation programmes. When To Get Medical AdviceSee a GP if you have persistent symptoms of COPD, particularly if youre over 35 and smoke or used to smoke. There are several conditions that cause similar symptoms, such as asthma, bronchiectasis, anaemia and heart failure. A simple breathing test can help determine if you have COPD. Find out more about tests for COPD. While theres currently no cure for COPD, the sooner treatment begins, the less chance there is of severe lung damage. Find out more about how COPD is treated. Page last reviewed: 20 September 2019 Next review due: 20 September 2022 Via https://www.knowyourasthma.com/are-asthma-and-copd-the-same-thing/ How Can I Deal With Stress During The Covid
Asthma CAN Kill – Make an Asthma Action Plan
Even though the number of COVID-19 cases have gone down, nearly everyone is still experiencing stress because of the pandemic. Some also are concerned as more activities return and businesses increase capacity and relax mask mandates. Stress can affect your well-being and quality of life. It can be an asthma trigger. Itâs important that you continue to take care of yourself during this time. Find some self-care practices that work for you. Some examples are:
The CDC also offers more information on coping with stress. When you have a chronic disease like asthma, taking part in a support group can have many benefits. AAFA has free online support groups for people with asthma and allergies. For support and encouragement through the COVID-19 pandemic, join the AAFA community. Viruses Can Trigger An Asthma AttackA viral infection can trigger an asthma attack, which will cause the airway to tighten, making it harder to breathe. If the attack is mild, asthma symptoms can be treated at home, but if the attack is more serious, a person with asthma may need emergency treatments. These treatments may include oxygen, antibiotics and medications administered through a nebulizer. If you experience severe symptoms, call 911 or go to the hospital. Hospitals are safe places to go for care. Delaying emergency care for any reason, including coronavirus fears, can make your condition worse or even be life-threatening. Learn more about in an emergency. Antibiotics do not kill viruses, so they cannot cure COVID-19, but a doctor might prescribe antibiotics if a bacterial infection is also present in the lungs. Signs Of Uncontrolled AsthmaMost deaths from asthma come from uncontrolled asthma. Make sure your asthma is always well controlled by having your child on the correct preventative medications. Seeing an asthma specialist such as pulmonologist or allergist can also help, Parikh said. Signs of uncontrolled asthma can sneak up on you, so be sure to know the symptoms of it: waking up at night, using your quick relief inhaler more than twice a week, needing oral or injected steroids one to two times per year, coughing, wheezing, shortness of breath all of these are signs your asthma is not controlled, she said. There are two types of medicine: quick relief and long-term control. Have A Plan If You Get SickDetermine who could assist you if you were to get sick and had to , and look for a way to have medications and food delivered to your home. UMMS provides our expert-reviewed content to keep our community informed. When sharing this copyrighted content, please link to our site so that critical updates are reflected. In This Section: What Are Oral And Intravenous Corticosteroids For Asthma Methylprednisolone , prednisone , and prednisolone may need to be prescribed when inhaled medications fail to control asthma. Examples of such situations include after an acute asthma attack or when a respiratory infection or allergy aggravates asthma symptoms. How corticosteroids workCorticosteroids decrease the inflammation within the airway passages that contributes to asthma symptoms and acute attacks. Who should not use these medications
UseDrug or food interactionsUse caution with other drugs that suppress the immune system, such as cyclosporine . Phenobarbital , phenytoin , or rifampin may decrease the effectiveness of corticosteroids. Some drugs, such as ketoconazole or erythromycin , may increase blood levels and toxicity of corticosteroids. An increased risk of stomach bleeding may occur when taken with high-dose aspirin or with blood thinners such as warfarin . Corticosteroids tend to increase blood glucose levels in individuals with diabetes, so diabetic therapy, such as insulin or oral medicines, may need to be adjusted. Talk to your doctor or pharmacist before taking other medications with oral corticosteroids. Side effectsRisk Factors For AsthmaSeveral risk factors have been associated with asthma mortality, including a history of near-fatal asthma requiring intubation and mechanical ventilation, hospitalization or emergency care visit for asthma in the past year, currently using or having recently stopped using oral corticosteroids , not currently using inhaled corticosteroids, a history of psychiatric disease or psychosocial problems, poor adherence with asthma medications and/or poor adherence with a written asthma action plan, food allergy in a patient with asthma . Near-fatal asthma and fatal asthma represent the most severe clinical presentations of asthma. Near fatal asthma is described as acute asthma associated with a respiratory arrest or arterial carbon dioxide tension greater than 50 mmHg, with or without altered consciousness requiring mechanical ventilation . In the NFA the most important pathophysiological events that lead to death are cardiac arrhythmias and asphyxia followed by complications of invasive mechanical ventilation such as barotrauma and ventilator-associated pneumonia. In a study of asthma patients admitted with a near-fatal episode, two-thirds of subsequent severe attacks or deaths occurred within 1 year of the previous life-threatening admission . It was observed that the prevalence of sensitisation to moulds increased with increasing severity of asthma . Several factors were identified as contributing factors in asthma deaths . What Are Anticholinergic Inhalers For AsthmaIpratropium bromide , tiotropium , and umeclidinium are used with beta-agonists for severe symptoms. How anticholinergic inhalers workThese drugs decrease bronchospasm and secretion of mucus in airways and are often used with albuterol to enhance effectiveness. In general, they are not as effective as the beta-agonists in treating asthma. These medications work by blocking receptors that cause spasm. Who should not use these medications
UseBoth handheld inhalers and a solution for use with a nebulizer are available. Many inhaled products have specific devices and you should be thoroughly informed on how to use the inhaler or nebulizer prescribed for you. These drugs are typically used three to four times per day. Drug or food interactionsSince anticholinergic inhalers have little or no effect beyond the area applied, they are unlikely to interact with other drugs. Side effectsAnticholinergic inhalers are not indicated for acute asthma attacks. The most common adverse effect is dry mouth. Individuals with glaucoma should be closely monitored by their ophthalmologist. Will My Wheezing Or Coughing Be WorseNot necessarily. You might be surprised to learn that you may not have more of these than usual during a severe asthma attack. So donât judge how bad your asthma attack is based on how much you wheeze or cough. In fact, very severe asthma attacks may affect your airways so much that you donât get enough air in and out of your lungs to make a wheezing sound or cough. Does My Child Need To Wear A Mask
How To Treat An Asthma Attack | What To Do During An Asthma Attack | Inhaler Treatment At Home
COVID-19 vaccinations are now available in the U.S. for everyone 12 years old and older. Children in this age range should get vaccinated as soon as possible so they are protected from COVID-19. Children should continue to wear a face mask and stay 3 feet apart in all public spaces, including schools if they are:
Children with a disability that keeps them from safely wearing a mask and children under 2 should not wear masks. What Is Asthma AnywayFirst up, a little anatomy refresher: Your airways, which extend between your nose and mouth and your lungs, have the very important job of carrying air in and out of your body, according to the National Heart, Lung, and Blood Institute . When you have asthma, triggers like animal fur, pollen, mold, cold air, cigarette smoke, exercise, and respiratory infections like colds cause your airways to get inflamed, according to the NHLBI. That inflammation can cause swelling, which in turn can prompt the muscles around your airways to tighten, making it hard to get air in and out. At the same time, your airways might also expel more mucus than they usually do, making it even harder to breathe. Experts dont know exactly what causes some people to get asthma when others dont, but its pretty safe to assume that its probably a combination of environmental factors and genetic factors. For example, if someone in your immediate family has asthma, youre more likely to have it too, according to the Centers for Disease Control and Prevention . Beyond that, the general cause is a stronger-than-normal response from your immune system to certain triggers, which is why you get all that inflammation when people without asthma dont, says the NHLBI. So What Are The Symptoms You Should Watch Out ForWhich signs of asthma you might experience differs from person to person and some are more common than others, Raymond Casciari, M.D., a pulmonologist at St. Joseph Hospital in Orange, California, tells SELF. Its possible that youll have such a mild reaction to one of your personal asthma triggers that you dont take much note of it. But if the effects get worse, they can turn into an asthma attack, which is a potentially life-threatening exacerbation of asthma symptoms. Thats why its so important to know the common signs of asthma, including the more subtle ones. These are classic asthma signs you should know:
Management Of Acute Asthma Exacerbations
5 Symptoms of Low Blood Oxygen (Hypoxia)
SUSAN M. POLLART, MD, MS; REBEKAH M. COMPTON, MSN, FNP-C; and KURTIS S. ELWARD, MD, MPH, University of Virginia Health System, Charlottesville, Virginia Am Fam Physician. 2011 Jul 1;84:40-47. Patient information: See related handout on how to treat an asthma attack, written by the authors of this article. In 2005, the prevalence of asthma in the United States was nearly 8 percent , and approximately 4 percent of Americans experienced an asthma attack., There have been many advances in medical therapy to prevent the worsening of asthma symptoms, including an improved understanding of asthma etiology, identification of risk factors for asthma exacerbations, and evidence supporting the benefits of written asthma action plans. In persons older than two years with asthma, neither the injectable nor the intranasal influenza vaccine increases the likelihood of an asthma exacerbation in the period immediately following vaccination. However, one study of infants found an increase in wheezing and hospital admissions after intranasal influenza vaccination. Seasonal influenza vaccine does not reduce the risk of developing an asthma exacerbation. Influenza vaccination appears to improve asthma-related quality-of-life in children during influenza season. Monitoring Asthma At HomeSome people use a handheld peak flow meter to evaluate their breathing and determine when they need intervention, before their symptoms become severe. People who experience frequent, severe asthma attacks should know how to reach help quickly. Peak expiratory flow can be measured using a small handheld device called a peak flow meter. This test can be used at home to monitor the severity of asthma. Usually, peak flow rates are lowest between 4 AM and 6 AM and highest at 4 PM. However, more than a 30% difference in rates at these times is considered evidence of moderate to severe asthma. People with moderate to severe asthma, particularly those who need daily treatment to control symptoms, often use a peak flow meter to take measurements and compare them to their personal best to help identify signs of worsening asthma or the onset of an asthma attack. All people with asthma should have a written treatment action plan that was devised in collaboration with their doctor. Such a plan allows them to take control of their own treatment and has been shown to decrease the number of times people need to seek care for asthma in the emergency department. How Is Hypoxia And/or Hypoxemia Diagnosed ChartIn general, an individual patients hypoxemia is usually diagnosed by oxygen monitors placed on fingers or ears and/or by determining the oxygen level in a blood gas sample . Normal readings are about 95% to 100% oxygen saturation levels; generally, oxygen is supplied if the level is about 92% or below. Blood Oxygen Levels Chart Using a Pulse Oximetry
The treatment for hypoxia and/or hypoxemia is to give additional oxygen to the patient and into the body as quickly as possible, especially if cerebral hypoxia is suspected, or to treat the underlying cause of the hypoxia. Many patients will respond to additional oxygen supplied by a nasal cannula. The quicker the oxygen level reaches normal, the better the prognosis is for the patient. However, the timing is very important, because cerebral hypoxia can occur within a few minutes and, in many patients, may not be reversible. Some patients may be treated in a hyperbaric chamber that increases oxygen concentrations in the blood , while others may require mechanical ventilation with oxygen supplied at higher than normal atmospheric concentrations. Others, such as mountain climbers or airline passengers, may need only additional oxygen provided by oxygen masks until they reach lower levels where oxygen concentrations are closer to the normal levels in the atmosphere. However, care must be used when giving oxygen, as it can be toxic to tissues if it is used excessively . Hyperoxia may cause: How Does Heart Failure Affect Oxygen SaturationOxygen saturation is a term used to define how much oxygen the hemoglobin in your blood is carrying. It is commonly measured by a pulse oximetry monitor, a non-invasive device that attaches to the end of your finger. When people with stable COPD also have heart failure, it is not unusual for them to experience shortness of breath, yet have a normal oxygen level reading. In fact, people with both COPD and heart failure could have an oxygen level 96, which would normally be considered high oxygen levels for a COPD patient, and still experience shortness of breath. This is because, as the volume of blood pumped by the heart lessens, the oxygen saturation level is not immediately affected. However, the lower volume of blood being pumped means that your organs are getting less oxygen. Over time, lack of oxygen affects every organ in the body including the lungs, which may eventually lower oxygen saturation./1 Care Advice For Asthma Attack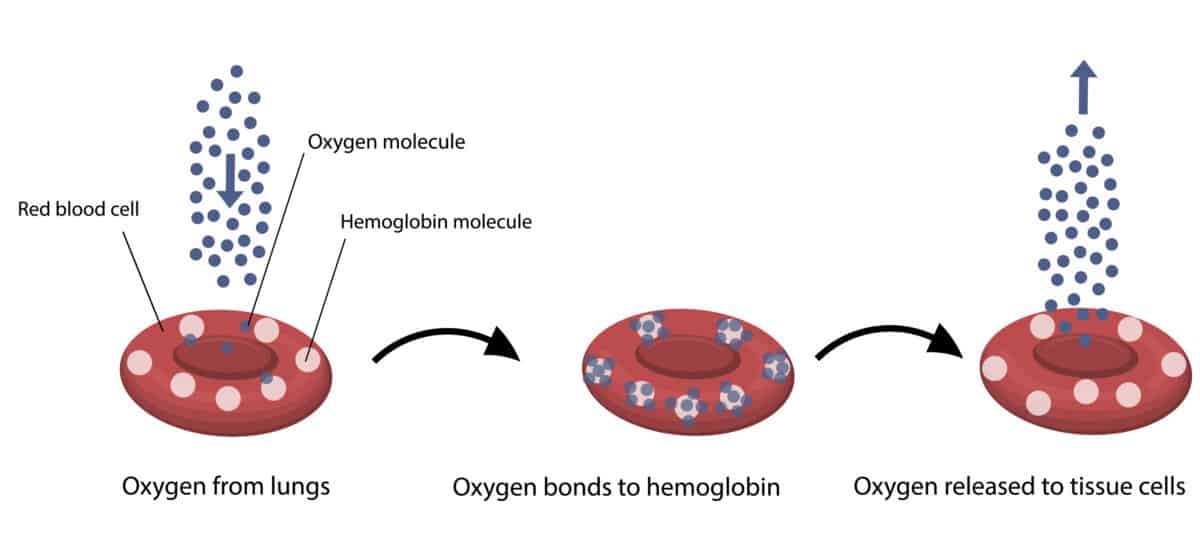
What Does The Control Pause Mean
100 People Hold Their Breath for as Long as They Can | Keep it 100 | Cut
If your CP is less than 10 seconds then: Asthma symptoms are severe. Breathlessness, wheezing and/or coughing will be frequently present throughout the day and at night. Relative breathing volume as determined by such a low breath hold is very big. If your CP is less than 20 seconds then:
If your CP is between 20 and 40 seconds then:
If your CP is greater than 40 seconds then:
Essential rules to make progress: Three steps to increasing your CP: STEP 1 Stop Big Breathing: a. Close Your Mouthb. Stop Sighing swallowc. Apply gentle calm breathingd. Never hear your breathing during rest STEP 2 Take physical exercise with correct breathing. Control Pause as a determinant of carbon dioxide tolerance For Those With Asthma What Is Normal Breathing
Asthma is usually characterized by coughing, sometimes wheezing, and often shortness of breath. Many people with asthma are used to having difficulty breathing or “breathing abnormally.” But what does it mean to experience normal breathing, especially with asthma? We asked some of our contributors at Asthma.net to share their thoughts. Here is what they had to say: What To Do During A SpellDont panic. Lie the child on their side and observe them. Dont shake the child, put anything into their mouth or splash water onto them. Keep their head, arms and legs away from hitting anything hard or sharp. Allow the episode to stop by itself. Treat the child normally after the event. Do not punish or reward the behaviour. What Can Be Done In The MeantimeNo special treatment is needed. Anti-epileptic treatment is not effective and is rarely recommended or trialed. Oral iron supplementation may have a role in reducing the frequency and severity of breath-holding spells, particularly if iron-deficiency anaemia is present . Treating anaemia, if present, will often decrease the frequency of spells which lead to passing out. Supportive management are generally all that is needed during an episode. The parents’ most important job is to not reinforce the breath-holding behaviour through a reward of excessive care and attention. Know your childs signs of tiredness and make sure they get plenty of rest. Help your child feel secure by minimising and managing their frustration. It is important that your child is not treated in any special way or differently from their siblings or other children. Behavioural problems can outlast the period of time that spells occur and become more of a burden to the family. Ask your doctor for help and/or referral to a behaviour modification or positive parenting program, usually run by your local community health centre. Contact Doctor During Office Hours
People Cant Die From AsthmaSadly, when an asthma attack occurs without proper care, death can occur. Ten Americans die every day due to asthma. Most of the deaths happen due to lack of oxygen supply and not because of a cardiac arrest. Hence, it is important to note that providing timely oxygen supply to asthmatic patients can avert deaths. In fact, a life-threatening asthma attack actually indicates an increase in the chance of them occurring again. Breathing Exercises For AsthmaBreathing exercises for asthma can be broadly divided into three groups: exercises aimed at manipulating the pattern of breathing ; exercises aimed at increasing the strength and/or endurance of the respiratory muscles ; and exercises aimed at increasing the flexibility of the thoracic cage and improving posture . In this article, we will focus on breathing retraining techniques, because these currently have the strongest and most convincing evidence base for effectiveness in asthma and are the most widely practiced. It should be noted that although many practitioners are applying these techniques clinically to children and teenagers, the only robust current research trial evidence applies to adults, with a recent Cochrane search for evidence in other age groups finding zero papers for inclusion in their review . Breathing retraining for asthma is a specific area of breathing exercise therapy that, after several years of relative neglect, has seen a considerable resurgence in research activity over the last decade. The breathing training techniques most frequently investigated have been physiotherapist-administered breathing exercises , as well as alternative techniques, such as the Buteyko breathing method and yogic breathing . Of these, physiotherapy and Buteyko have the higher level of evidence and are now mentioned in several guidelines for asthma management. Asthma Management Can HelpA single individual’s asthma does not necessarily remain in the same category permanently. A person with seasonal asthma triggers may find that at a certain time of year for instance, when ragweed pollen is in the air he or she is in a higher severity group than during the rest of the year. Asthma that starts during childhood also may become less severe as a person grows and his or her airways become wider. For any person with asthma, effective ongoing asthma control can help them move into a less severe category. The asthma experts at UI Health can help you bring your asthma under control. To request an appointment, please fill out the online form or call 312.996.3300. How Is Asthma Diagnosed
How Long Can I Hold My Breath?
To diagnose asthma, a doctor will do a physical exam and ask about the person’s medical history, including whether anyone else in the family has asthma. The doctor might do tests like spirometry or peak flow meter tests. These involve blowing into devices that can measure how well the lungs are working. Allergy tests or exercise tests can tell doctors if asthma is brought on by allergens or physical activity. Doctors may use X-rays to rule out other problems. Asthma Patients Reduce Symptoms Improve Lung Function With Shallow Breaths More Carbon Dioxide
Asthma patients taught to habitually resist the urge to take deep breaths when experiencing symptoms were rewarded with fewer symptoms and healthier lung function, according to a new study from Southern Methodist University, Dallas. The findings are from a large clinical trial funded with a grant from the National Institutes of Health’s National Heart, Lung, and Blood Institute. The results suggest asthma patients using behavioral therapy in conjunction with their daily asthma medicine can improve their lung health over the long-term, said principal investigators Thomas Ritz and Alicia E. Meuret, both SMU clinical psychologists. Also, sufferers may potentially reduce their dependence on emergency medication, such as rescue inhalers, the researchers said. Asthma can be a life-threatening disease if not managed properly, according to the American Lung Association. Nearly 26 million Americans have asthma, says ALA. One of the most common chronic disorders in childhood, asthma is the third leading cause of hospitalization among children under 15, ALA says. Story Source: Introduction: The Need For Innovations In Asthma Management StrategiesAmong the outstanding achievements of modern medicine are the remarkable improvements in asthma outcomes occurring over the latter part of the last century. Although the prevalence of asthma has risen , improvements have occurred in hospitalisation, mortality, symptom control and quality of life . These were achieved through the widespread use of safe, effective medication and structured, proactive care . Hospital-based specialist care is now reserved for those with poor control or severe, therapy-resistant disease while generalists and primary care clinicians now provide care for the majority with mild or moderate disease. It is possible that an inappropriate sense of complacency arose, with a feeling that we had got on top of asthma, and asthma slipped down in priority in the health agenda. Can You Die From Holding Your BreathYes, but not if youre above water. When you black out, your body automatically starts breathing again. Your lungs will gasp for air since youre programmed to inhale and exhale, even if youre unconscious . If youre underwater, the gasp for air may let in a huge volume of water. Inhaling water isnt always fatal if youre resuscitated by or have the water pumped out of your lungs by emergency responders. But in most cases, blacking out underwater from holding your breath is deadly. When Should You Call A Doctor For An Asthma Attack If you think you or your child may have asthma, make an appointment with your health care provider. Some clues pointing to asthma include the following:
If you or your child has asthma, you should have an asthma action plan worked out in advance with your health care provider. This plan should include instructions on what to do when an asthma attack occurs, when to call the health care provider, and when to go to a hospital emergency department. The following are general guidelines only. If your provider recommends another plan for you, follow that plan.
Although asthma is a reversible disease, and treatments are available, people can die from a severe asthma attack. If you are in the emergency room, treatment will be started while the evaluation is still going on. Asthma Disrupts Normal BreathingResponse from Lorene Alba, AE-C: During normal breathing, air enters the body when you inhale through your nose or mouth. This air travels down your airways into your lungs and air sacs. The airways are open and clear, allowing air to flow in and out easily. When you have asthma, the airways become narrow from swelling on the inside and muscle tightening on the outside, while excess mucus clogs the airways. The air becomes trapped in the air sacs and cannot get back out through the narrow airways.3 Paying attention to how you are breathing when you have asthma can help with symptoms. First, try to always inhale through your nose; this helps warm and filter the air before it goes into your lungs. Practice breathing from your belly instead of your chest. This helps get more oxygen to your bloodstream and helps you relax. Its easy:4
Natural Selection And Evolution
Asthma (Medical Definition) | Quick Overview
Mutations alter an organism’s genotype and occasionally this causes different phenotypes to appear. Most mutations have little effect on an organism’s phenotype, health, or reproductive . Mutations that do have an effect are usually detrimental, but occasionally some can be beneficial. Studies in the fly suggest that if a mutation changes a protein produced by a gene, about 70 percent of these mutations will be harmful with the remainder being either neutral or weakly beneficial. studies the distribution of genetic differences within populations and how these distributions change over time. Changes in the in a population are mainly influenced by , where a given allele provides a selective or reproductive advantage to the organism, as well as other factors such as , , , and . Over many generations, the genomes of organisms can change significantly, resulting in . In the process called , selection for beneficial mutations can cause a species to evolve into forms better able to survive in their environment. New species are formed through the process of , often caused by geographical separations that prevent populations from exchanging genes with each other. Causes And Inciting Factors Of Asthmatic EpisodesAsthmatic episodes may begin suddenly or may take days to develop. Although an initial episode can occur at any age, about half of all cases occur in persons younger than 10 years of age, boys being affected more often than girls. Among adults, however, women are affected more often than men. When asthma develops in childhood, it is often associated with an inherited susceptibility to allergenssubstances, such as pollen, dust mites, or animal dander, that may induce an allergic reaction. In adults, asthma may develop in response to allergens, but viral infections, aspirin, weather conditions, and exercise may cause it as well. In addition, stress may exacerbate symptoms. Adults who develop asthma may also have chronic rhinitis, nasal polyps, or sinusitis. Adult asthma is sometimes linked to exposure to certain materials in the workplace, such as chemicals, wood dusts, and grains. These substances provoke both allergic and nonallergic forms of the disease. In most of these cases, symptoms will subside if the causative agent is removed from the workplace. Know The Early Symptoms Of AsthmaEarly warning signs are changes that happen just before or at the very beginning of an asthma attack. These signs may start before the well-known symptoms of asthma and are the earliest signs that your asthma is worsening. In general, these signs are not severe enough to stop you from going about your daily activities. But by recognizing these signs, you can stop an asthma attack or prevent one from getting worse. Early warning signs of an asthma attack include:
If you have these warning signs, adjust your medication, as described in your asthma action plan. Viral Infection To PredispositionThe fact that early-in-life sensitization to multiple allergens carries the greatest risk for developing asthma brings the question of what factors result in a predisposition to this phenotype. Although infection with rhinovirus is the major cause of acute exacerbation, in those genetically at risk of asthma, rhinovirus-induced wheezing in the first three years in the life is also the greatest risk factor for developing asthma at 6 years of age . Impaired TLR3-mediated IFN- and – production by asthmatic epithelial cells would make susceptible to both viral infection and allergic sensitization . Reduced primary IFN production by lower-airway epithelial cells enables some viruses to replicate, leading to cytotoxic cell, release of inflammatory products and enhanced viral shedding. Such events provide a strong stimulus for recruitment of immature DCs and their priming for allergen sensitization . When asthmatic epithelial cells are received to damage by rhinovirus infection, the cells generate increased amounts of the pro-Th2 cytokine thymic stromal lympoietin , which stimulates DCs and increases allergic inflammation, whereas exogenous IFN-b applied to asthmatic epithelium exerts anti-Th2 as well as antiviral properties . What Should Be Done During The Attack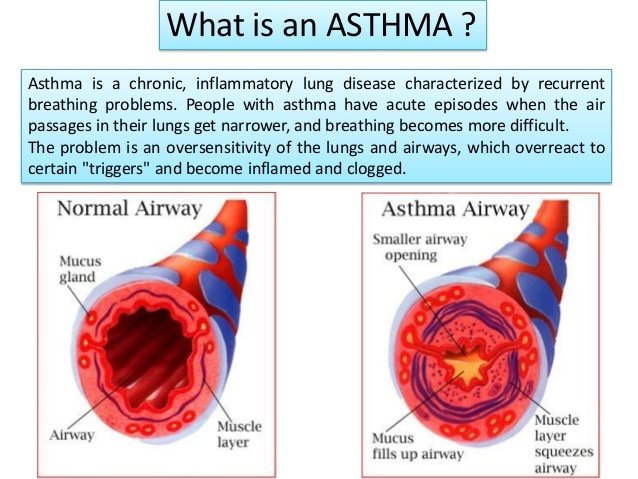 People with asthma should have an action plan for dealing with an acute attack. In general, it is important to stay calm and take prescribed medications. Quick-relief medications, including, rapid-onset inhaled beta2-agonist bronchodilators, such as albuterol, are used to treat asthma attacks and are taken on an as-needed bases. They relieve symptoms rapidly by relaxing the muscles surrounding the airways, helping to open the bronchial tubes. More severe attacks may require systemic corticosteroids to reduce airway mucus and swelling. Global Alliance Against Chronic Respiratory DiseasesThe Global Alliance against Chronic Respiratory Diseases contributes to WHOs work to prevent and control chronic respiratory diseases. GARD is a voluntary alliance of national and international organizations and agencies from many countries committed to the vision of a world where all people breathe freely. What Is An Asthma AttackAn asthma attack is the episode in which bands of muscle around the airways are triggered to tighten. This tightening is called bronchospasm. During the attack, the lining of the airways becomes swollen or inflamed, and the cells lining the airways make more and thicker mucus than normal. All of these things — bronchospasm, inflammation, and mucus production — cause symptoms such as trouble breathing, wheezing, coughing, shortness of breath, and trouble with normal daily activities. Other symptoms of an asthma attack include:
An asthma attack can get worse quickly, so it’s important to treat these symptoms right away. Without immediate treatment, such as with your asthma inhaler or bronchodilator, it will become harder to breathe. If you use a peak flow meter at this time, the reading will probably be less than 50% of your usual or normal peak flow reading.. Many asthma action plans suggest interventions starting at 80% of normal. As your lungs continue to tighten, you wonât be able to use the peak flow meter at all. Your lungs will tighten so there is not enough air movement to make wheezing. You need to go to a hospital right away. Unfortunately, some people think that the disappearance of wheezing is a sign of improvement and donât get emergency care. What Can Be Done About ItAsthma can be controlled. Moreover, it can be controlled by those who have asthma. The role of the physician is to provide the means for the patient to control asthma and to teach the patient to use provided measures . Since asthma varies greatly in pattern of symptoms and severity, the treatment plan needs to be individualized. This should be done in a systematic manner. Goals of therapy must be realistically attainable and explicitly defined for you. The plan for attaining the treatment goals must be understood. Once the measures needed for control of asthma are identified, they can be placed in the hands of the patient with appropriate instructions for usage. Parental supervision is needed for young children, but progressive responsibility for self-management is given with advancing maturity. Treatment may consist of medication, environmental changes, and life-style changes. The more the patient understands the disease and its treatment, the better the outcome is likely to be. The patient should therefore be an active partner in making decisions about treatment. Be wary, however, of superstitions and misinformation regarding asthma. More than almost any other medical problem, asthma is associated with a wide diversity of medical and nonmedical opinion. Both the physician and the patient therefore need to exercise judgment. Four common sense measures to remember are: Reducing The Burden Of Asthma
What is Asthma? – Dr. Hirennappa B Udnur
Asthma cannot be cured, but good management with inhaled medications can control the disease and enable people with asthma to enjoy a normal, active life. There are two main types of inhaler:
People with asthma may need to use their inhaler every day. Their treatment will depend on the frequency of symptoms and the different types of inhalers available. It can be difficult to coordinate breathing using an inhaler especially for children and during emergency situations. Using a spacer device makes it easier to use an aerosol inhaler and helps the medicine to reach the lungs more effectively. A spacer is a plastic container with a mouthpiece or mask at one end, and a hole for the inhaler in the other. A homemade spacer, made from a 500-ml plastic bottle, can be as effective as a commercially-manufactured inhaler. Access to inhalers is a problem in many countries. In 2019, only half of people with asthma had access to a bronchodilator and less than one in five had access to a steroid inhaler in public primary health-care facilities in low-income countries . How Do Healthcare Providers Diagnose AsthmaYour healthcare provider will review your medical history, including information about your parents and siblings. Your provider will also ask you about your symptoms. Your provider will need to know any history of allergies, eczema and other lung diseases. Your healthcare provider may order a chest X-ray, blood test or skin test. Your provider may order spirometry. This test measures airflow through your lungs. Environmental Remediation For AsthmaThe medical management of asthma and treatment of acute attacks has improved substantially, but the prevalence of asthma continues to rise in urban settings in industrialized Western countries. There is still controversy about the hygiene hypothesis, and it is not yet clear that early exposure to certain antigens could be exploited as a preventive measure. Given what is known about asthma, avoidance of asthma trigger factors would be expected to at least reduce the frequency and severity of symptoms. EPA recommendations for an “Asthma Friendly House” are shown in the iFrame below. EPA Recommendations Asthma Friendly House For additional measures, also see the EPA Home Environment Checklist. There is some evidence that interventions to reduce dust, animal dander, mold, and exposure to cockroaches are effective, but the literature indicates that allergen reduction is difficult to achieve and the effectiveness is not as great as expected. The four articles cited below suggest that environmental remediation interventions that target one or two potential targets are of limited, if any value. However, they suggest that multifaceted interventions can reduce symptoms, school absences, and hospital visits for acute asthma care. From the Abstract: Results Summary: From the Abstract: “Evidence synthesis Summary How Is Asthma DiagnosedAsthma is diagnosed based on symptoms, physical examination, and lung function tests.14 Your health care provider will ask about the type and frequency of symptoms and what you were doing when the symptoms started. Additionally, your provider may do a test called spirometry. This test checks how much and how quickly you can exhale air. It is possible for a person with a history of asthma symptoms to have normal spirometry results.1 In this case, your health care provider may suggest a methacholine challenge. Methacholine is an inhalable spray that is especially irritating to people with asthma. It triggers airway narrowing and allows your provider to measure how sensitive your airways are. The methacholine challenge is best for ruling out asthma, although the results are not always conclusive. The test also helps to differentiate asthma from other lung conditions. People whose airways do not narrow after inhaling methacholine are very unlikely to have asthma. Finally, other tests may be used to figure out what subtype you have. Is It Possible To Outgrow It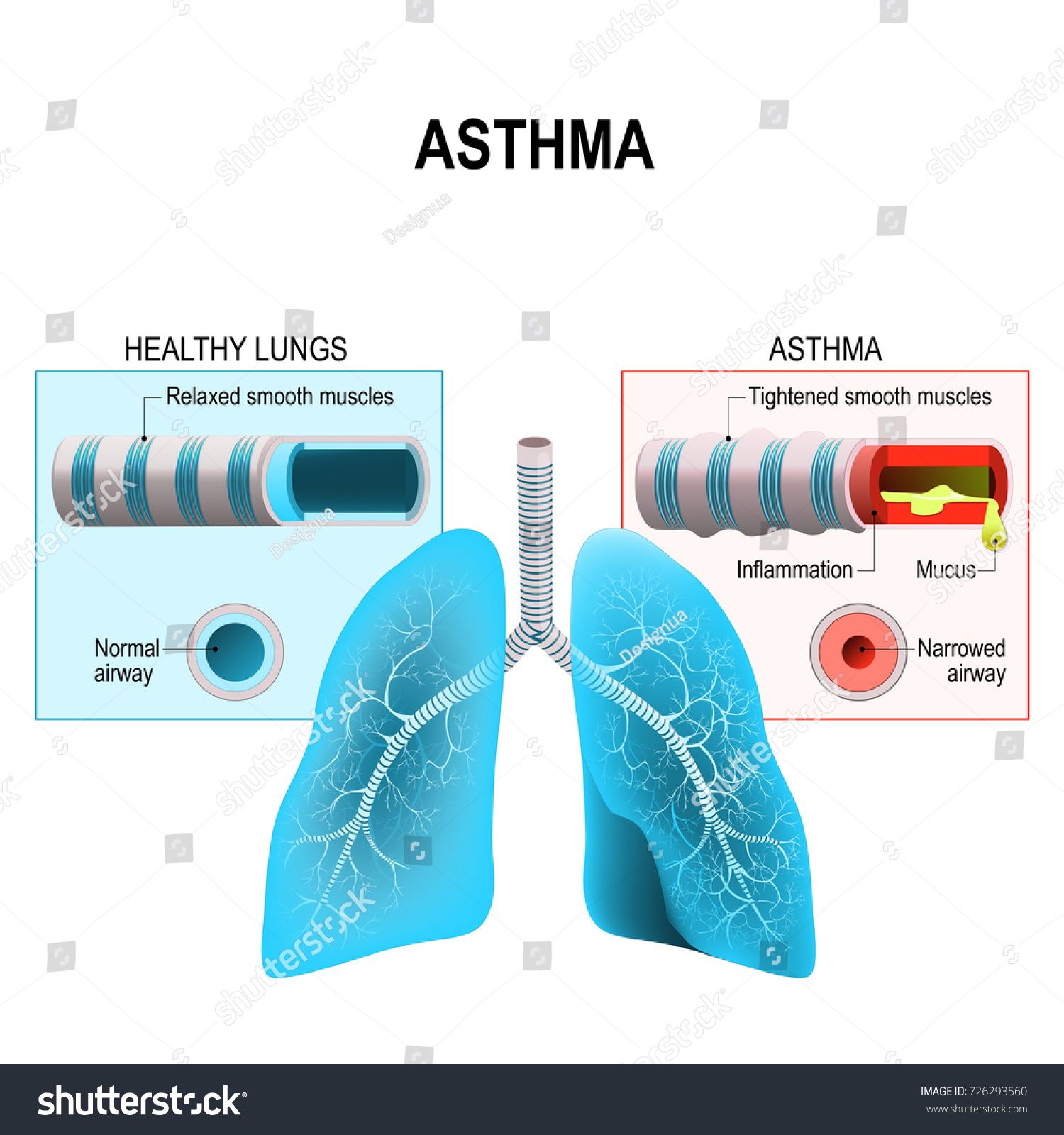 Asthma is a long-term disease. You may feel better for months, but generally, the airways remain inflamed and sensitive. Some children do seem to “outgrow” their symptoms.1 However, other children need to continue taking medications to control their asthma. In one study, 64% of people with mild childhood asthma symptoms did not have symptoms as adults.6 However, only 15% of people with severe childhood asthma were symptom-free in adulthood. It is not possible to predict who will outgrow their symptoms. What Is Asthma Characterized By4.9/5AsthmaAsthmacharacterized There are many different types of asthma, brought on by many different triggers.
Similarly, what causes a person to develop asthma? Asthma triggersExposure to various irritants and substances that trigger allergies can trigger signs and symptoms of asthma. Airborne substances, such as pollen, dust mites, mold spores, pet dander or particles of cockroach waste. Respiratory infections, such as the common cold. In this regard, what are the hallmarks of asthma? The classic signs and symptoms of asthma are shortness of breath, cough , and wheezing . Many patients also report chest tightness. What are the 4 types of asthma? Medical professionals rank asthma into four types from mild to severe.These types include: What Is Type 2 Inflammation In AsthmaAs many as 50-70 percent of asthma patients have a form of asthma characterized by Type 2 inflammation. Type 2 inflammation is a type of systemic allergic response that can result in increased asthma exacerbations and decreased lung function. Cytokines, which are proteins that signal the bodys cells and begin an immune response, are major contributors to Type 2 inflammation. Common asthma biomarkers are also present in Type 2 inflammation. These include:
When there are too many eosinophils in the blood, there is an increased risk of severe asthma flares. Learn more about eosinophilic asthma at eosasthma.org. Genetics also appear to play a role in Type 2. Studies show that if one or both parents have Type 2 inflammation related to asthma, their child is four times more likely to have asthma or an allergic disease. Regulation Of The Pulmonary Circulation Helps Restore The Ventilation/perfusion RatioPulmonary circulation depends on the pulmonary vascular resistance , gravity, alveolar pressure, and the hydrostatic pressure gradient provided by the right heart. The PVR, in turn, is influenced mainly by two factors: the inflation of the lung and the reaction of the arterioles to the partial pressure of oxygen in the blood. The PVR, which determines blood flow, is affected by three separate variables: the alveolar gas pressure that compresses the capillaries, the resistance of alveolar vessels , and resistance of extraalveolar vessels. Unlike the systemic circulation, the capillaries in the lungs accounts for about 40% of the PVR. At lung volumes greater than the FRC, capillaries are stretched and compressed, and the resistance of the alveolar vessels increases. At lower lung volumes, the extraalveolar vessels are not held open by their tethers to the alveolar tissues, and their resistance increases. These effects contribute to a biphasic relationship between PVR and lung volume. The PVR is minimum around the functional residual capacity, FRC. When To See A Doctor
What is Asthma? (The Sound of Wheezing)
If asthma is well controlled and you follow your treatment plan, you may be able to postpone worsening symptoms. However, asthma can get worse over time. Thats why its important to maintain regular check-ups with your doctor. If you think your asthma symptoms are occurring more frequently before youre scheduled for your next appointment, go ahead and make a new appointment. Its important to stay on top of changes in asthma symptoms so you can control them. Asthma Causes And TriggersWhen you have asthma, your airways react to things in the world around you. Doctors call these asthma triggers. They might cause symptoms or make them worse. Common asthma triggers include:
When Asthma Is Not Just Asthma: Type 2 InflammationNews, Asthma, Severe Asthma News & Updates Asthma was once considered a single, though complex, disease. Now its recognized as a spectrum of diseases. Genetic and environmental factors play a role in airway inflammation and hyper-reactivity. This leads to common asthma symptoms: coughing, wheezing and shortness of breath. Severe asthma is one form of the disease. Its estimated that 5-10 percent of people with asthma have severe asthma. Severe asthma is the diagnosis when
Recent medical breakthroughs involving severe asthma are transforming how its diagnosed and treated. Airway inflammation is a particular focus. Effect Of Interventions On Natural History Of AsthmaTwo recent studies addressed the possibility that ICSs may prevent the putative declines in lung function believed to occur shortly after the beginning of the disease in adults who have late-onset asthma. A retrospective study reported the results of an observational study of adults who had mild-to-moderate asthma and were treated for 5 years with an ICS. One group, treated early in the disease , had better outcomes in terms of lung function than those who started treatment more than 2 years after diagnosis. The group in which treatment was started more than 2 years after diagnosis, however, had lower levels of lung function at the beginning of the trial. Therefore, it is not possible to determine from these data what the results would have been in a randomized trial. Two recent long-term observational studies report an association between ICS therapy and reduced decline in FEV1 in adults who have asthma . However, long-term RCTs will be necessary to confirm a causal relationship. Who Strategy For Prevention And Control Of Asthma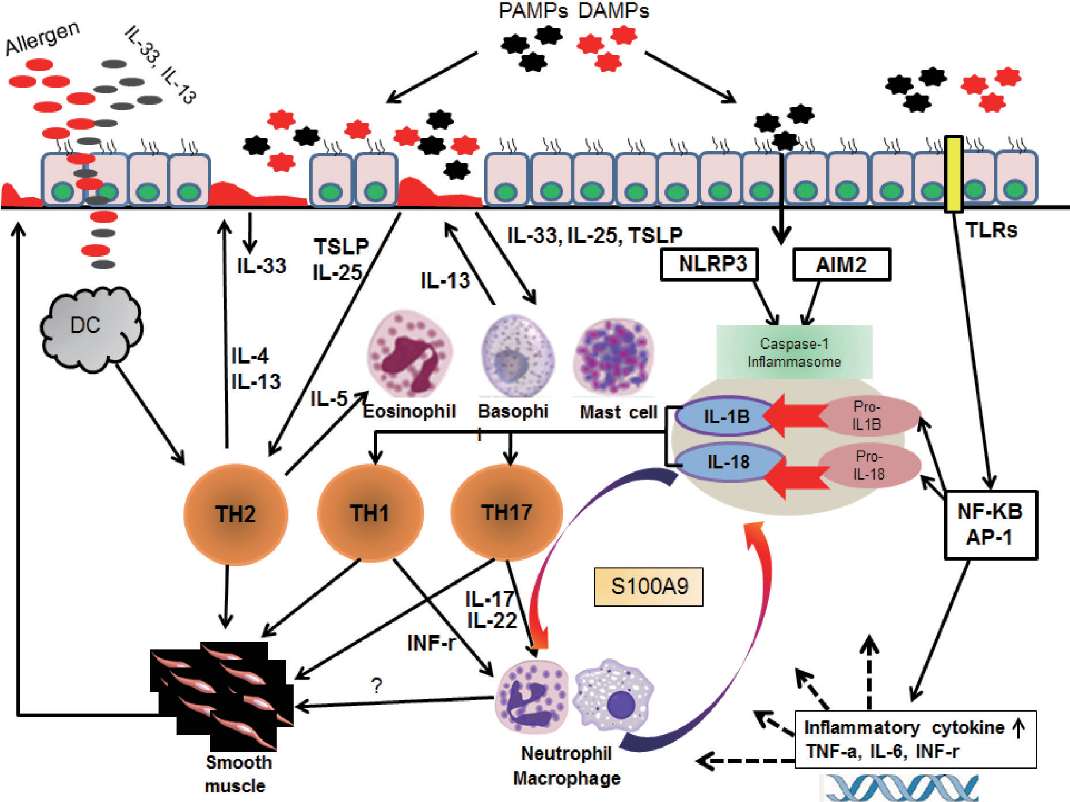 Asthma is included in the WHO Global Action Plan for the Prevention and Control of NCDs and the United Nations 2030 Agenda for Sustainable Development. WHO is taking action to extend diagnosis of and treatment for asthma in a number of ways. The WHO Package of Essential Noncommunicable Disease Interventions was developed to help improve NCD management in primary health care in low-resource settings. PEN includes protocols for the assessment, diagnosis, and management of chronic respiratory diseases , and modules on healthy lifestyle counselling, including tobacco cessation, and self-care. Reducing tobacco smoke exposure is important for both primary prevention of asthma and disease management. The Framework Convention on Tobacco Control is enabling progress in this area as are WHO initiatives such as MPOWER and mTobacco Cessation. Know The Symptoms Of An Asthma AttackAn asthma attack is the episode in which bands of muscle surrounding the airways are triggered to tighten. This tightening is called bronchospasm. During the attack, the lining of the airways becomes swollen or inflamed and the cells lining the airways produce more and thicker mucus than normal. All of these factors — bronchospasm, inflammation, and mucus production — cause symptoms such as difficulty breathing, wheezing, coughing, shortness of breath, and difficulty performing normal daily activities. Other symptoms of an asthma attack include:
The severity of an asthma attack can escalate rapidly, so it’s important to treat these asthma symptoms immediately once you recognize them. Without immediate treatment, such as with your asthma inhaler or bronchodilator, your breathing will become more labored. If you use a peak flow meter at this time, the reading will probably be less than 50%. Many asthma action plans suggest interventions starting at 80% of normal. As your lungs continue to tighten, you will be unable to use the peak flow meter at all. Gradually, your lungs will tighten so there is not enough air movement to produce wheezing. You need to be transported to a hospital immediately. Unfortunately, some people interpret the disappearance of wheezing as a sign of improvement and fail to get prompt emergency care. Diagnostic Criteria And Therapeutic Interventions In The Elderly With AsthmaExisting pharmacological therapies that are frequently utilized to treat and manage asthma include inhaled corticosteroids, -agonists, and anti-IgE antibodies . Non-allergic asthma, which is more frequent in the elderly population, is less responsive to corticosteroids . Total serum IgE measurement was initially thought to be a reliable indicator of asthma since many asthmatic patients are allergic and it might distinguish asthma from COPD during the diagnostic work-up . However, it has been recognized that not all asthmatic patients are allergic. Furthermore, elderly patients tend to have lower IgE levels due to immunosenescence thus making the clinical diagnosis difficult using this method . Much of the research that has investigated asthmatic biomarkers has excluded the elderly population. Thus, further studies are necessary in order to understand the effect of aging and immunosenescence on the expression of biomarkers that may be utilized in the clinical diagnosis of asthma . How Do You Monitor Asthma SymptomsMonitoring your asthma symptoms is an essential piece of managing the disease. Your healthcare provider may have you use a peak flow meter. This device measures how fast you can blow air out of your lungs. It can help your provider make adjustments to your medication. It also tells you if your symptoms are getting worse. Key Points: Definition Pathophysiology And Pathogenesis Of Asthma And Natural History Of Asthma
Asthma | Clinical Presentation
|
AuthorEverything you wanted to know about asthma. In one place Archives
November 2022
Categories |

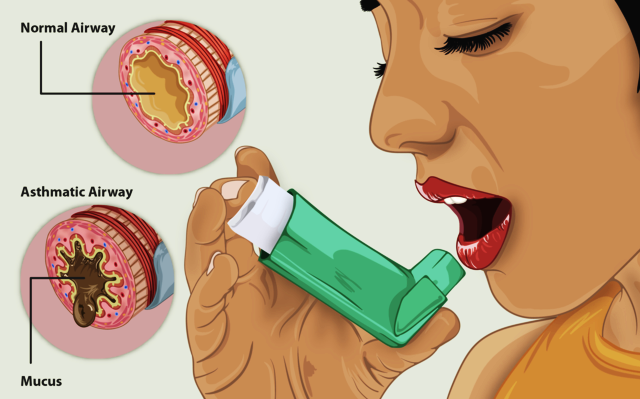


 RSS Feed
RSS Feed
